This report will take around 14 minutes to read. During that time, 20 American lives will have been lost to Covid-19.
Americans are dying who didn’t need to be.
Welcome back to Week 34 in my weekly reports analyzing the Covid-19 pandemic and its effects on the country and higher education. For those of you reading this on my blog, Off the Silk Road, I have also launched a newsletter, where these reports can be sent directly to your email each week. Click here to subscribe.
Last week, we looked at the country’s possible paths coming out of the Thanksgiving holiday. This week, we will analyze the alarming trends as hospitalizations and deaths are rising and at record highs.
A national look
“The pandemic nightmare scenario—the buckling of hospital and health-care systems nationwide—has arrived.…Hospitals are becoming overwhelmed, causing them to restrict whom they admit and leading more Americans to needlessly die.”
This is an excerpt from The Atlantic’s piece on America’s record-high hospitalizations — over 101,000 Americans are currently hospitalized for Covid-19. 1 in every 5 people in America’s hospitals is hospitalized for Covid-19 — never before has one ailment affected such a large proportion of the hospitalized population. While hospitals may be able to add extra beds, staff are contracting this disease and are unable to take care of patients. Dr. Ashish Jha at the Brown University School of Public Health noted that the proportion of cases being hospitalized is falling. This is likely because in order to triage, the bar for admission into hospitals has been set higher. As a result, Americans are likely dying of COVID-19 either at home or in the hospital because they are unable to seek adequate care at full hospitals. The American Ambulance Association said this week that America’s 911 system is at a breaking point.
Overflowing hospitals do not just impact Covid-19 patients. This means that people may die of strokes, heart attacks or other causes at home. While in the spring hospitals could easily shift personnel between different parts of the country, healthcare workers being needed everywhere makes it impossible to do so now. This week, the Institute for Health Metrics and Evaluation at the University of Washington said that Covid-19 was the leading cause of death in the U.S. this week, surpassing heart disease.
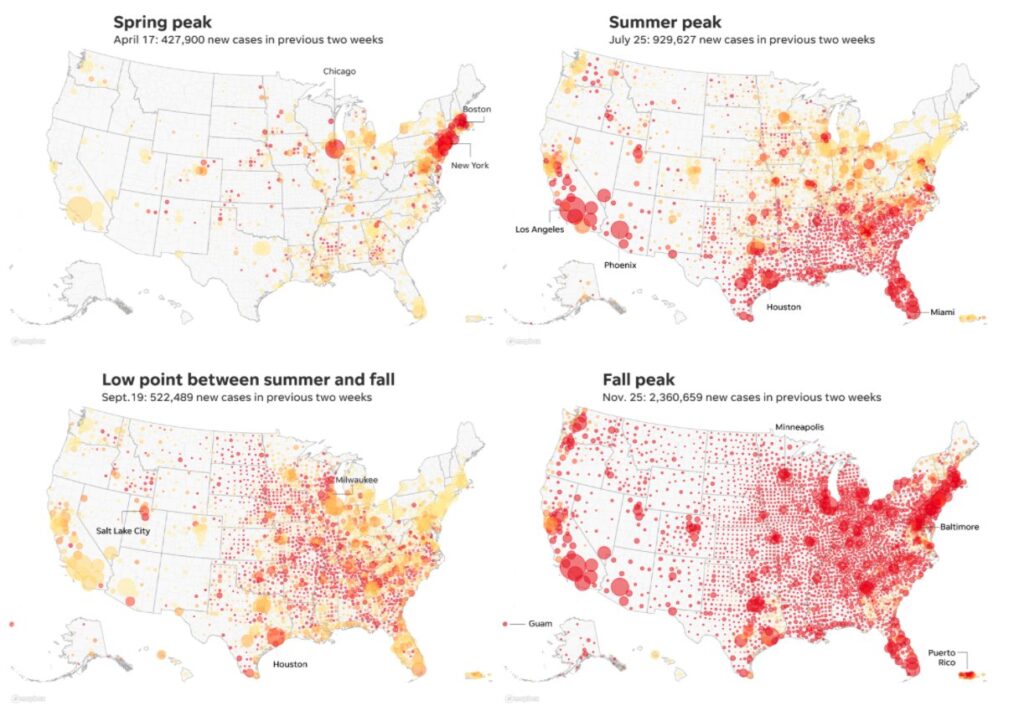
Yes, the vaccine is coming. Yes, a new president is coming. But it won’t be enough. This week, CDC director Dr. Robert Redfield said the next few months of the Covid-19 pandemic will be among “the most difficult in the public health history of this nation.” Perpetuating a raging pandemic when a vaccine is on the way is like having a house that’s on fire with the fire trucks on the way, but you decide to light another match anyway. Public health strategies such as contact tracing are failing to keep up with ever-rising cases, which have now topped 200,000 multiple days this week and will continue to rise after we fully feel the effects of the Thanksgiving surge. Deaths are now starting to follow the trajectory of the 1918 flu pandemic. Those who may have been infected from Thanksgiving are only starting to feel sick now, and many will check into hospitals and sadly will never return home. This all comes as a new Pew poll reports that more than half of Americans know someone personally who has been hospitalized or died from Covid-19. Infectious disease specialist Dr. Jeremy Faust notes that “as of November 28th, there have been more deaths among Americans *age 40 and under* directly attributed to Covid-19 (4,674) than died as a result of the entire Iraq War (4,424).” This week, an American died from Covid-19 every 43 seconds. (CNN’s Christi Paul held 43 seconds of silence on New Day on Saturday.) Those who watch the Johns Hopkins coronavirus dashboard know the cycle: the deaths reset in the morning, are counted through the day and will only stop at midnight. By then, the death toll reaches a large portion of those who have died during 9/11. It is only a matter of days until the daily death toll will likely exceed 3,000. Hospitals have been lining up iPads for the sick to say goodbye to their loved ones.

This week, the CDC issued a report to all Americans with 10 basic health strategies (this list is adapted from Dr. Craig Spencer’s Twitter thread):
- Universal face mask use
- Maintaining physical distance from other persons and limiting in-person contacts
- Avoiding non-essential indoor spaces and crowded outdoor spaces
- Increasing testing to rapidly identify and isolate infected persons
- Promptly identifying, quarantining, and testing close contacts of persons with known Covid-19
- Safeguarding persons most at risk for severe illness or death from infection with SARS-CoV-2, the virus that causes Covid-19
- Protecting essential workers with provision of adequate personal protective equipment and safe work practices
- Postponing travel
- Increasing room air ventilation and enhancing hand hygiene and environmental disinfection
- Achieving widespread availability and high community coverage with effective Covid-19 vaccines
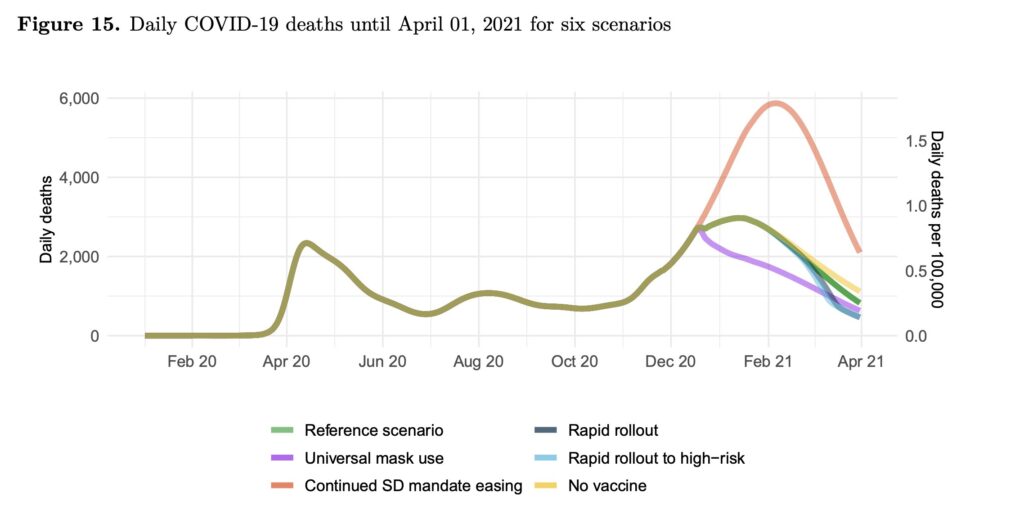
It is up to all of us to follow these strategies, and here’s why. The latest IHME modeling shows that even if rapid rollout of a vaccine is accomplished (blue line), the most effective way of lowering the daily death count is with universal masking, as mass vaccination results may not be felt until March or April. Although a vaccine rollout at the projected pace will have some effect, possibly preventing 11,000 deaths, wearing a mask is expected to save 66,000 lives by April 1. Think of a vaccine as a weak bicycle brake: it will slow the pandemic but will not stop it when a runaway train is going off a cliff.
The U.S. has recorded over 1 million cases in the first five days of December alone. There were more Covid-19 cases in the U.S. in the month of November alone than January through June combined. It’s not a rural or urban problem anymore; it’s an American problem, fueled by incompetent leadership and a defiance by a significant portion of the population who “refuse to wear a piece of cloth on their face to protect one another,” as state in the obituary for Dr. Marvin J. Farr written by his son.
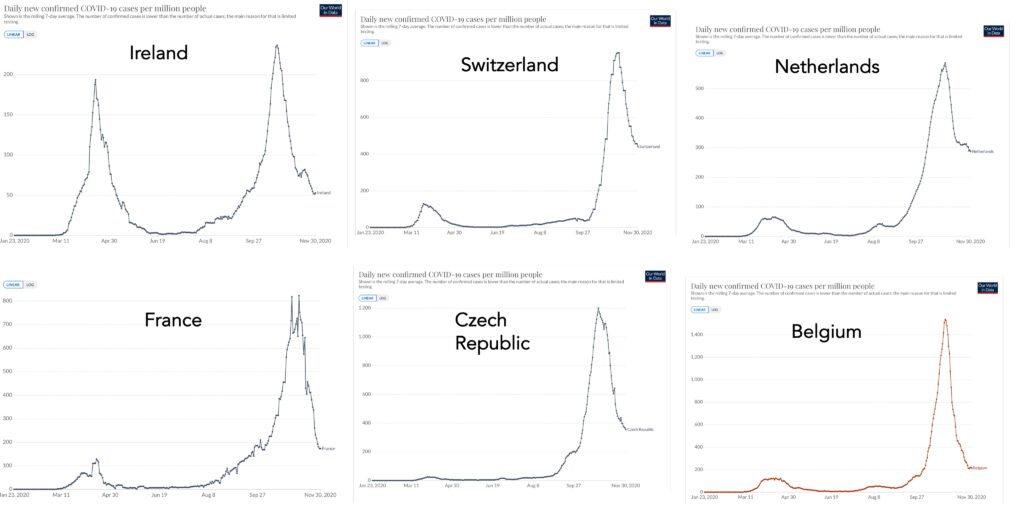
We can control this pandemic without a vaccine; other countries in Europe have done so, despite fall surges. America has chosen the path that will involve mass deaths over the next few months, even as many Americans will continue to travel over the holiday season. Yes, for the betterment of human lives Dr. Scott Atlas has left the White House. He leaves behind a legacy of the deliberate killing of thousands of American lives. The president, however, has worked harder to destroy our democracy and overturn the results of a free and fair election than to save American lives.
It is not just a federal issue; it is a failure of states to communicate accurate public health information to their residents. An analysis I conducted earlier in the week shows that only 13 states only held one Covid-19 press briefing for the whole month of November and one state (Florida) held none. Many of the states that have been hit the hardest throughout the month, such as the Dakotas and Wyoming, have held incredibly few briefings. The mean number of briefings in November Democratic governors held was 5.04, while that same figure for Republican governors was 3.27.
We have not yet begun to feel the effects of the Thanksgiving surge. An NPR analysis shows that while many Americans did stay home, 13% still traveled a significant distance.
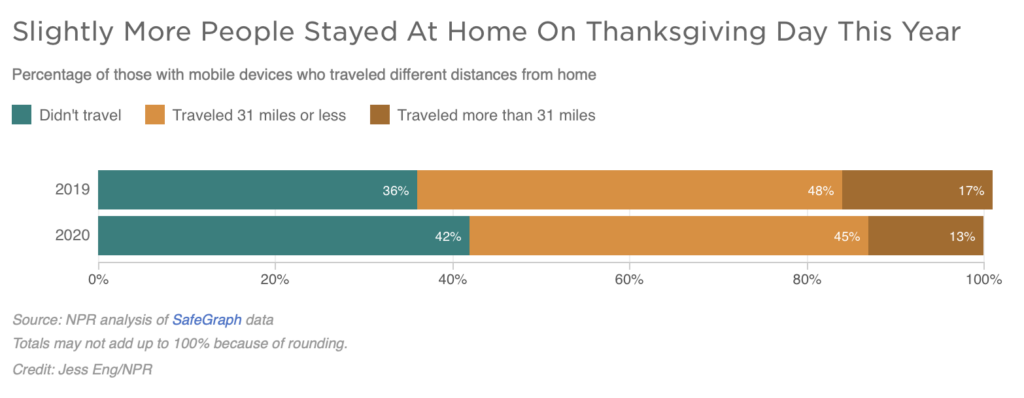
We are approaching the winter with a baseline that is too high for our healthcare system to handle, and despite highly efficacious vaccines being just around the corner, it is likely that cases will continue to increase. We simply do not know when this peak will occur.
Let’s take a look at some of the latest scientific developments:
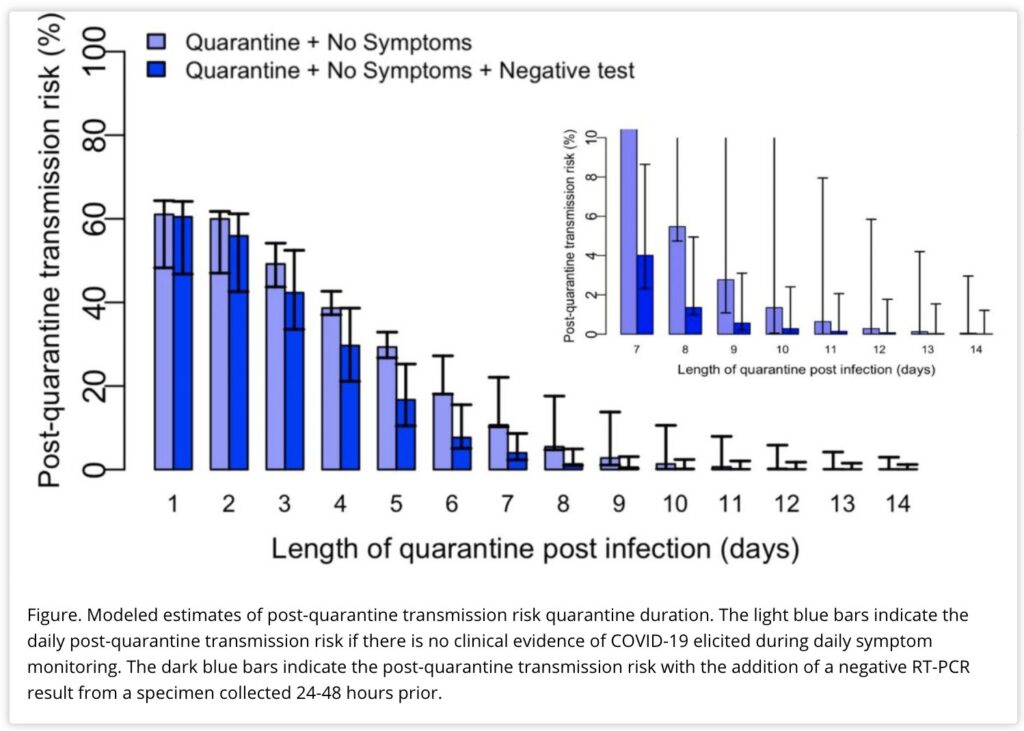
- The CDC announced this week that while the 14-day quarantine for close contacts is the best way to reduce risk, 7 or 10 days are possible with a negative test upon leaving quarantine. This is due to modeling that shows a low chance of transmitting the virus after 7 days. It has also received criticism from health experts, who have said that the CDC should work to create services such as food delivery or wage compensation that can support those in quarantine or isolation.
- According to a new CDC study of samples from blood banks, the new coronavirus infected people in the U.S. in mid-December 2019, though virologists question the study’s limitations.
- A new meta-analysis shows that people with Covid-19 are most contagious from 2 days before symptoms and for 5 days after, suggesting that the isolation period may be shortened.
- An analysis showed that testing over 80% of its population over a matter of weeks reduced daily case counts in Slovakia by over 80% “almost immediately.” However, experts have said that such a strategy would not be feasible in the U.S., primarily due to the fact that the highest regional positivity rate in Slovakia was 4.8% and the same figure for the U.S. is 50%.
- A study published in The Lancet estimated that preventative measures among the homeless population in England might have avoided 21,092 infections, 266 deaths and 1,164 hospital admissions.
- A study from Germany published in PNAS found that after 20 days of a mask mandate infections were reduced by 45%, with zero economic cost.
- In Korea, a diner at a restaurant infected others that he was not in direct contact with, drawing attention to aerosol transmission and the risks of indoor dining.
- A preprint found a correlation between the lifting of eviction moratoriums and increased Covid-19 incidence and mortality.
- An analysis Florida data scientist Rebekah Jones published found that within Florida students, “the state-wide case incidence rate in districts without mask mandates (12.7 per 1,000 students enrolled face-to-face or hybrid) was 38% higher than those who attended in-person within districts that did have mask mandates.”
- A preprint published by University of Colorado scientist Dan Larremore and colleagues found that a test based on loss of smell could be a cheaper and effective alternative for detecting possible Covid-19.
- Odd study of the week: A preprint found that among a survey of residents in Chicago, 21% of respondents (n=835) reported an increase in rat sightings around their homes during the stay-at-home order and increased rat sightings were positively associated with proximity to restaurants, low-rise apartment buildings, and rat feces in the home.
Finally, some news on vaccines. The FDA is expected to approve Pfizer’s vaccine on December 10 and Moderna’s vaccine on December 17.
- The UK approved Pfizer’s vaccine for emergency use this week.
- The CDC’s Advisory Committee on Immunization Practices issued the recommendation for the first vaccine doses to be allocated to healthcare workers and residents of long-term care facilities. Despite supply chain obstacles, Operation Warp Speed officials anticipate 20 million people will be able to be vaccinated in December, another 30 million in January and 50 million in February. One official said that “100 percent of Americans that want the vaccine will have had the vaccine” by June.
- Americans will receive a card when they are vaccinated to remind them to come back for their second dose. This comes as 99% of pharmacies in the United States do not have access to a -80°C freezer, which will be necessary for storing Pfizer’s vaccine at a stable temperature.
- Maine has applied lessons from its lobster industry when it comes to acquiring dry ice.
- It is likely that children will not be able to get the vaccine until at least the summer due to a current lack of clinical trials.
- Bloomberg has set up a tracker tracking global vaccine allocations.
- According to a Pew research study, the share of Americans who currently plan to get a Covid-19 vaccine has increased to 60%, but just 37% say they’d be comfortable being among the first groups of people to get a vaccine.
- There is an ongoing debate as to whether prisoners should be in the priority line for a vaccine.
- Former presidents Carter, Clinton, Bush and Obama all tell CNN they will get their vaccines on camera for the American public.
- This weekend, I launched a new dashboard that tracks local news reports and state press releases for allocation numbers for the first doses of Covid-19 vaccines. It is likely that the first Pfizer shipment will be distributed on December 15, followed by the first Moderna shipment a week later. Then, the second Pfizer shipment will arrive, followed by another Moderna shipment and a third Pfizer shipment before the end of the month. While each person will require two doses, the first shipment will consist of first doses for the priority populations (mostly distributed at hospitals and pharmacies for long-term care facilities). That group’s second doses will come in the future Pfizer shipments. The first Pfizer shipment is enough to vaccinate about 1% of the adult population once. It is likely that ~3.5% of each state’s adult population will be vaccinated by the end of the year (accounting for 2 doses/person).
Less than 1% of America’s population lives in long-term care facilities, but as of December 3, 2020, this tiny fraction of the country accounts for 39% of US Covid-19 deaths, according to the COVID Tracking Project. America has failed its elderly generation as the virus now continues to ravage through nursing homes. A state-by-state approach will no longer work as some states are quicker to react and impose stay-at-home orders than others. It’s not a question of lockdown vs. “freedom.” It’s an issue of saving American lives, and through targeted individual and community health approaches, we can attempt to mitigate some of the damage the coming weeks will bring.
Let’s move on to our discussion of higher education.
Higher education
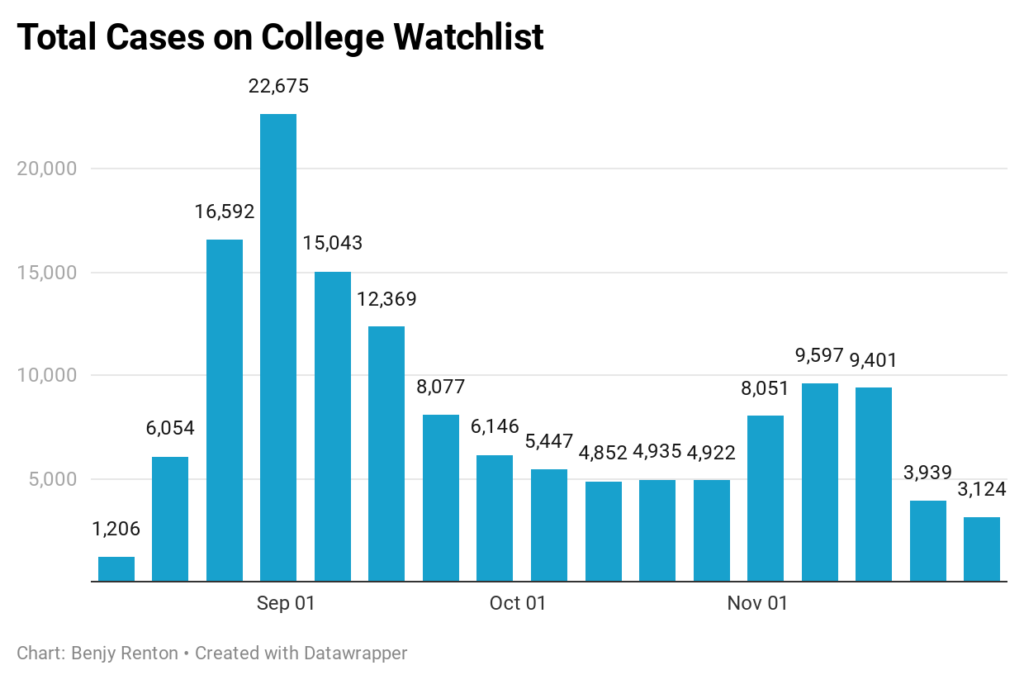
Each Friday, I update the College Watchlist, which is currently tracking 156,013 total cases at 96 colleges across the country. At the top of my list of cases in the last 7 days are:
- University of Illinois – 206
- University of Kentucky – 200
- San Diego State University – 176
- Brigham Young University – 167
- University of Arizona – 130
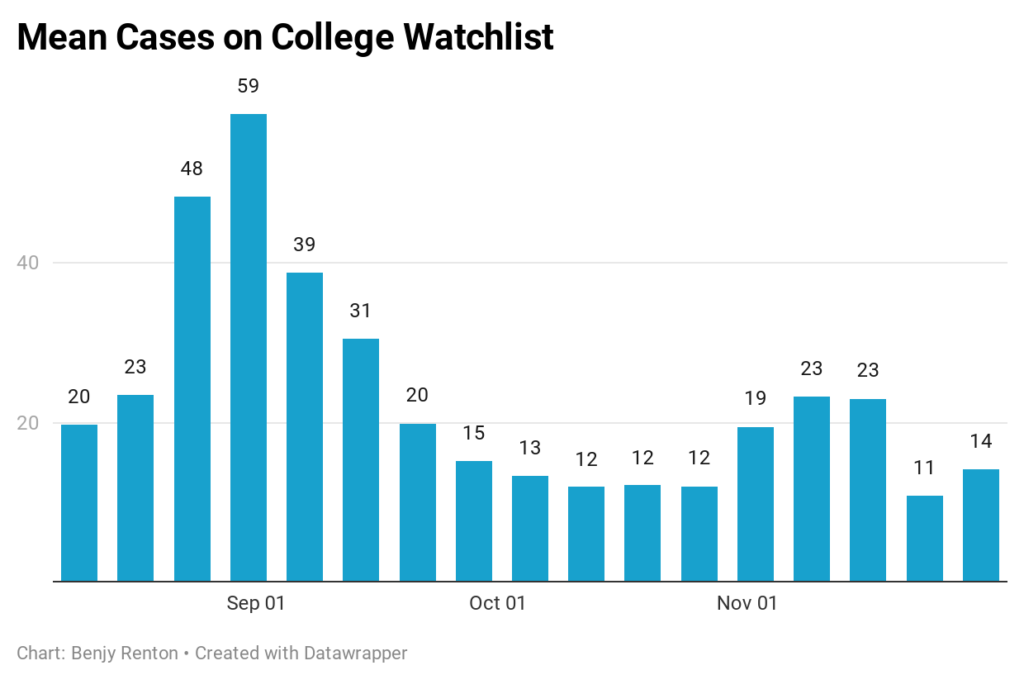
Many schools reported far fewer cases since most students are currently not on campus. However, for those that did report, some reported increases post-Thanksgiving (mean cases increased). There were 4,050 cases in the last 7 days among these colleges.
We are still in the process of analyzing strategies from the fall and I will update you on this research when it is published. However, in the meantime, The Chronicle of Higher Education’s Francie Diep offers five lessons about coronavirus on campus.
- With precautions in place, classrooms and other formal on-campus spaces aren’t important vectors of viral spread.
- Off-campus social gatherings are the top drivers of coronavirus at colleges.
- But wait, the spread isn’t entirely off campus. Take residence halls.
- Entry and surveillance testing are critical.
- College-student outbreaks can lead to infections and deaths among more vulnerable people.
Here’s a roundup of this week’s higher ed news:
- Washington Post columnist Lizette Alvarez implores colleges to devote more to mental health this spring. “There’s no drive-through swab for depression,” she writes. “Instead, struggles may be hidden away in quiet dorm rooms, as suffering students are unwilling or unable to share their pain on campuses that can feel, by necessity, like minimum-security prisons.”
- The Boston Globe’s Deidre Fernandes profiles the Broad Institute, whose high-throughput lab enabled many New England colleges to stay open this fall.
- According to The Chicago Tribune’s Elyssa Cherney, the University of Illinois has now conducted 1 million Covid-19 tests using its saliva-based technology at all three campuses.
- Harvard University aims to double the number of students living on campus next semester.
- The University of Florida has denied 144 professors the ability to teach remotely this spring, leaving some to feel as if university administration has put their safety at risk.
- “Given current conditions and UNC’s track record, the plans for spring are doomed to repeat too many of the failures of the fall,” faculty at the University of North Carolina write. “The only ethical decision is to cancel face-to-face instruction (with the exception of classes that demand it, such as clinical experience) and to keep on-campus residency reserved for those who have special circumstances.”
- “Perhaps if this country was able to implement the Wesleyan strategy on a larger scale, as well as create a culture of joint responsibility, this pandemic would ease its course and we might be able to prevent the next,” one Wesleyan University student writes.
- Higher Ed Dive covers the possibility of colleges distributing vaccines.
- “A deadly pandemic isn’t the time for gamesmanship,” The Michigan Daily’s Aria Gerson writes in her call for more public health transparency among the football team. “It’s the Wolverines’ responsibility to the Ann Arbor community to make sure any potential outbreak doesn’t spread.”
- All Claremont Colleges will stay remote for at least the start of the spring semester due to LA County guidelines [I suspect this may be more and more common as the weeks continue].
- Boston University’s contact tracing team details the basics of contact tracing on campus. As one contact tracer describes it, it’s a job that is “half-detective, half-therapist.” One tracer described a need for “empathy” in the process.
- A new survey from American Campus Communities, one of the largest student housing developers and providers in the United States, found students living on or near campus in college housing this fall benefitted academically and socially. It also determined that students closely followed coronavirus safety guidelines, as reported in Inside Higher Ed.
- The U Experience is slated to open next month in Texas, promising students a “normal” college experience sans masks and social distancing while students take online classes at their home institutions. As I wrote on Twitter this week, I am skeptical of this Fyre Festival-like idea. On college campuses, testing is just one component of a “Swiss cheese” strategy — masks and distancing are important, especially at this scale (i.e. more than a family, which can be kept in a “bubble”). Remember what happens when you only rely on testing? You get the White House. The founders of this campus claim that their protocol is similar to the NBA, but the NBA employed masks and other measures as well as frequent testing. What you’re essentially going to have is the equivalent of a cruise ship, long-term care facility or prison — it will be incredibly hard to keep a completely sealed bubble and I do not think this will work in January, when the pandemic will be raging.
Based on case studies from college campuses this fall, the National Academies of Sciences, Engineering, and Medicine issued best practices for testing and behavior strategies on college campuses. A quick summary of both documents is below.
On testing:
- Testing is one part of a comprehensive strategy
- Routine collection and analysis of data are necessary
- Positive tests should be isolated in hours (modeling assumes this)
- Compliance expectations should be communicated
On behaviors:
- Don’t focus on socially undesirable behaviors; focus on the common good
- Use trusted messengers with attention to risks and rewards
- Highlight positive aspects of behavior change
- Avoid repeating misinformation, even to debunk it
As colleges prepare for the spring, we must continue to learn from the fall. We also must note that many of the elements colleges may have taken for granted in their reopening plans this fall will not work for the spring due to extremely high levels of community transmission nationwide that are likely to persist into January.
The Good Stuff
Let’s roll the clips of the good stuff. In my usual tradition, I feature my favorite stories from the week. Here are my Top 14.
- Jeff Gerson was admitted to NYU Langone Tisch Hospital in mid-March with a high fever and a cough and was placed on a ventilator. Weeks later and released from the hospital, he sent a letter thanking the more than 116 hospital workers who attended to him when he was sick with Covid-19.
- The Huffington Post’s Jeffrey Young detailed Dr. Anthony Fauci’s incredibly busy daily schedule.
- 102-year-old Angelina Friedman lived through the 1918 flu pandemic and beat the coronavirus twice.
- The Atlantic published a series of gripping photos chronicling the latest surge in hospitals.
- In what is now known as the “Fauci effect,” the number of medical school applicants is up 18% this year over last year.
- The Philadelphia Inquirer published an in-depth investigation into the Four Seasons Total Landscaping press conference.
- TIME magazine named 15-year-old scientist Gitanjali Rao as its first Kid of the Year.
- A New York Times reporter took one of the world’s only active cruises, a three-day voyage to nowhere around Singapore.
- NPR profiled the Twitter and TikTok personas of the Biden grandchildren.
- Despite the pandemic, some music programs continue to thrive, albeit with safety precautions.
- The New York Times examined the first weeks of the pandemic in New York through the eyes of six individuals.
- The Olympic rings were reinstalled in Tokyo and lit up for the first time in months.
- One New York Times reader proposed to her partner through the Morning Briefing newsletter.
- The Washington Post and CNN published their selected pictures of 2020.
Conclusion
When President Donald Trump first addressed the nation as president on January 20, 2017 and swore to “preserve, protect and defend the Constitution of the United States,” he declared “this American carnage stops right here and stops right now.” Now, that same president is witnessing American carnage at an unprecedented scale and continues to spread disinformation and do absolutely nothing to stop it. America is running out of time to turn its trajectory around. More Americans are dying from Covid-19 than at any point in the pandemic. Although the first doses of a vaccine are expected to be delivered in under 10 days, widespread vaccination will not occur for months and many will die while waiting in line. There is a definite end to this pandemic; it is up to all of us to muster all our strength to save our healthcare workers and our fellow Americans’ lives. Deaths at a massive scale will most likely continue for the next few weeks, though our actions now can pave the way for a brighter future.
I’d like to thank all the student journalists with whom I have the pleasure of working. In the next weeks and months ahead, they will become vital in chronicling their colleges’ paths forward for the spring and beyond. Support their work by reading it.
My best to all for good health.
Like what you see? Don’t like what you see? Want to see more of something? Want to see less of something? Let me know in the comments. And don’t forget to subscribe to the weekly newsletter!
For more instant updates, follow me on Twitter @bhrenton.



2 Comments
Harry Goldhagen · December 6, 2020 at 1:59 pm
Great job documenting a terrible period, Benjy! Keep up the excellent work!
Jack O · December 6, 2020 at 9:25 pm
Another comprehensive and very well sourced round up. The detail and data in the vaccine tracker is very impressive.
Keep up the great work. I am able to navigate the complexity of our moment better
with the factual undergirding curated by dedicated folks like you.
Comments are closed.