Welcome back to Week 17 in my weekly reports analyzing the Covid-19 pandemic and its effects on the country, higher education and study abroad. For those of you reading this on my blog, Off the Silk Road, I have also launched a newsletter, where these reports can be sent directly to your email each week. Click here to subscribe.
Last week, we looked at more plans for a national reset and examined testing as our only key to open colleges. This week, we will discuss this “new phase” of the pandemic and look at why some colleges have decided to abandon their plans for an on-campus fall semester.
There’s a lot of material to go through (as per usual), so let’s get straight to it.
A national look
The theme of this week’s report is “Reality Check.”
On CNN’s “State of the Union” last Sunday, Dr. Deborah Birx said that we are “in a new phase” and that the virus is “extraordinarily widespread.” Later in the week, she warned nine cities and California’s Central Valley about an uptick in test positivity rates. First, the good news: The U.S. seems to have made a U-turn in its daily case count, now reporting from 50,000 and 60,000 cases each day. This is by no means where we need to be, but it’s still a start. What accounts for this U-turn? A few factors:
- A slowing down (for now) of cases in Texas, Arizona and California, once large hotspots (virologist Trevor Bedford has a good thread outlining a sort of “herd immunity” that has been achieved there).
- A slowdown in testing (this is the first week since March that the country has conducted less tests than the previous week). While this is alarming, some of it can be contributed to the recent hurricane that hit the East Coast.
“We just have to assume the monster is everywhere,” Ohio Governor Mike DeWine, who later in the week had a false positive test result, said in The Washington Post. How can we show that this is true? Let’s look at some maps. These two maps show the new daily cases at the end of March and at the end of July. While in March the virus was concentrated in a few hotspots, the virus is now everywhere.
Additionally, the growth in rural areas cannot be understated. This graph shows the daily case growth in metro counties (blue) and nonmetro counties (yellow). While there was an initial “wave” in urban areas in April, the virus has seen equal growth in rural and urban areas this past month.
“They are dying. That’s true. And it is what it is,” President Trump said in a jaw-dropping interview with Axios’ Jonathan Swan. The U.S. death toll has exceeded 1,000 a day for the past 11 days, occasionally approaching 1,400. Deaths are always a lagging indicator when compared to cases, and we are in the middle of a tragic wave of fatalities.
One of the current concerns with an extraordinary widespread pandemic is that the American people have now become complicit in deeming any number that does not break daily case records as “fine.” And that makes the virus hard to contain. Looking at this graph, which compares urban density to infections per capita, it is clear that rural states are not immune from the virus.
“Covid-19 is an assault on America’s body, and a referendum on the ideas that animate its culture,” The Atlantic’s Ed Yong writes in a formidable piece unpacking every failure of the American response. Want to know how little we’ve progressed in our response? On May 30, when SpaceX’s Crew Dragon launched, we were all watching in our houses. On August 2, when Crew Dragon landed, we’re still watching in our houses. Nothing has changed (probably of much surprise to the astronauts as well). Each week, we try to answer two simple questions: How did we get here? And where do we go from here? The answer to the latter is testing.
Let’s begin this week’s discussion on testing. It’s a fact that America’s PCR testing has failed. With results taking up to two weeks (in my case, it took 15 days), it is clear that our testing system does not work, or in the words of Bill Gates, it’s “completely garbage.” Scientists have now proposed a two-tiered testing system: antigen tests for screening and assurance, and PCR tests for confirmation. Antigen tests, which work by detecting specific proteins in people’s saliva or nasal passages, are different from PCR tests, which amplify viral RNA. They are less specific and often have a higher false negative rating, which means that they could show a negative when someone in fact has the virus. However, they do show great promise at identifying especially infectious individuals because they appear to perform better for individuals who are shedding more virus. These tests may therefore dramatically speed the cycle of testing/isolating/tracing by enabling the rapid identification of at least a subset of highly infectious individuals. Antigen tests are cheaper, can be done multiple times per week, are able to run with saliva or a nasal swab, and may even be available at the point of care (homes, schools, workplaces) in weeks or months. In the absence of a national testing strategy, seven governors have banded together to procure antigen tests in large quantities. While you do trade speed with accuracy, models, such as this one by biologist Dr. Carl Bergstrom, show that frequency is key. “Even if you miss somebody on Day 1,” said Omai Garner, director of clinical microbiology in the U.C.L.A. Health System in The New York Times. “If you test them repeatedly, the argument is, you’ll catch them the next time around.” The UK has procured fast 90-minute tests that can detect flu and Covid-19 in one, so it is clear that these sorts of tests are possible. Now it’s just a question of developing them and scaling them up. Antigen tests, while not a perfect solution due to their accuracy, could be a key strategy for schools and colleges to reopen.
Across the nation’s K-12 schools, just one major school district — New York City — is attempting to offer some form of in-person instruction for the start of the academic year. The United States has a much higher number of cases per capita than any other country that has opened schools, according to the Kaiser Family Foundation. As President Trump continues to push for schools to reopen, his own son’s school will start the year with virtual learning. Without federal support for safety precautions, or making an effort to bridge the Internet gap for millions of students, schools are facing extreme hardships to reopen. “It’s like telling American families ‘we need you to jump out of a plane’ and then refusing to pack our parachutes or teach us how to use them correctly,” CNN’s Brianna Keilar said. For the schools that have already reopened, some students have tested positive and many others have quarantined. An alarming photo of a hallway crowded by mostly maskless students in a Georgia high school just shows the challenges of opening schools nationwide. “The question is not ‘When should we open schools?” ER doctor Jeremy Faust asks. “It’s ‘How long do we want them to stay open.’” Many schools in college towns will not open for in-person classes; the Ann Arbor school district (where the University of Michigan is located) has said it will watch for infection trends with the university before it decides to start in person. “The United States is reopening many of the wrong schools,” education professor Susan Dynarski said in The New York Times. “For colleges, competition for tuition dollars is pushing them to take outsize risks to get students back on campus, while for public school districts, inadequate funding — combined with the failure of government to curb the coronavirus — is keeping them from getting children safely back into school buildings.” According to a recent survey of teachers in a school district in Portland, Maine, 28% said they would return to school if public health officials said it was safe to do so, compared to 60% this past spring. Much of our discussion in recent weeks has not included boarding schools, which I liken to a bridge between K-12 and higher education due to the residential aspect. Loomis Chaffee, one of the most prestigious boarding schools in Connecticut, has moved Fall Term 1 online for boarding students, citing testing availability and risks of spread in a residential setting. Maybe these actions taken by boarding schools could affect colleges in similar areas.
As usual, more studies have been published and new information is now available to help us better understand Covid-19. Let’s take a look at some of the highlights:
- T-cell immunity found in some people who may have had prior exposure to other coronaviruses, such as the common cold, could explain why some people have protection against Covid-19.
- An NIH trial has begun for monoclonal antibodies, which could shorten time for recovery in the outpatient setting. This could be a promising treatment for mild or moderate Covid-19.
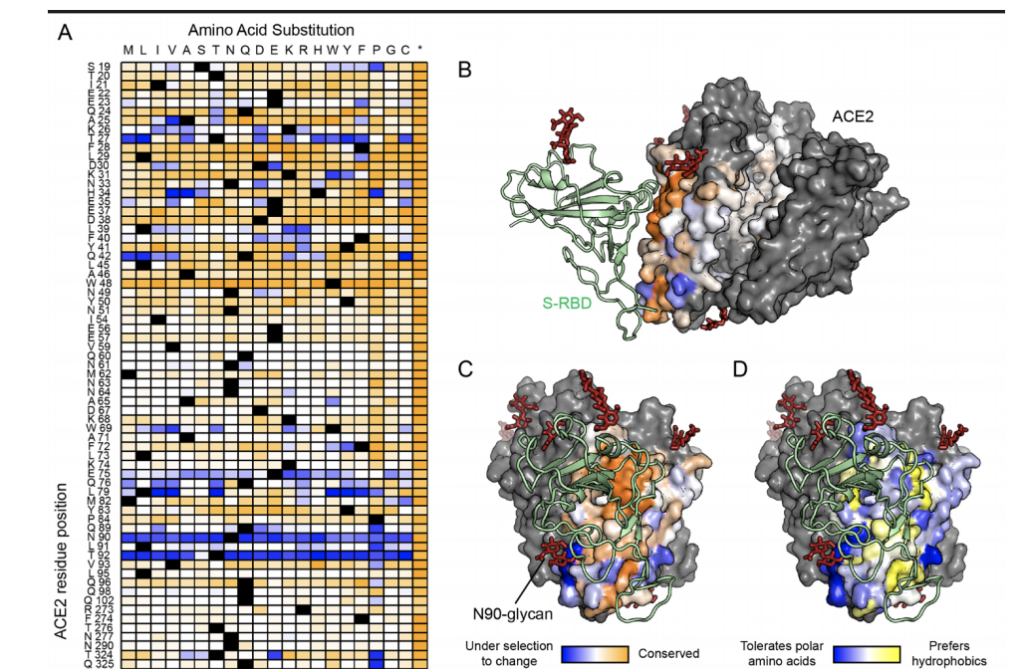
- Since SARS-CoV-2 binds to the ACE2 protein receptor, scientists have found a potential therapy — giving patients soluble ACE2 as a decoy. While this is in its early stages, the science is wildly impressive, not to mention the schematic.
- Researchers in The Lancet found a threefold increased risk of reporting a positive Covid-19 test and predicted Covid-19 infection in healthcare workers in the UK and U.S.
- A new study from Anne Wyllie at Yale found that the virus’ RNA is stable in saliva samples across a range of temperatures, meaning that ordinary collection devices can be used for mass saliva testing.
- This New York Times explainer underscores the fact that symptoms from Covid-19 are not just respiratory.
- A study from Italy (in Italian) found Italy’s overall Covid-19 seroprevalence (detection of antibodies) to be 2.5%, with the highest seroprevalence in the Lombardy region, at 7.5%. Notably, among those who tested positive for antibodies, 41.7% lived with someone else who was also infected, highlighting transmission within the family.
- From May 1 through June 30, 15 cases of methanol poisoning were reported in Arizona and New Mexico, associated with swallowing alcohol-based hand sanitizers, resulting in 4 deaths. It’s almost like someone said, “And then I saw the disinfectant…”
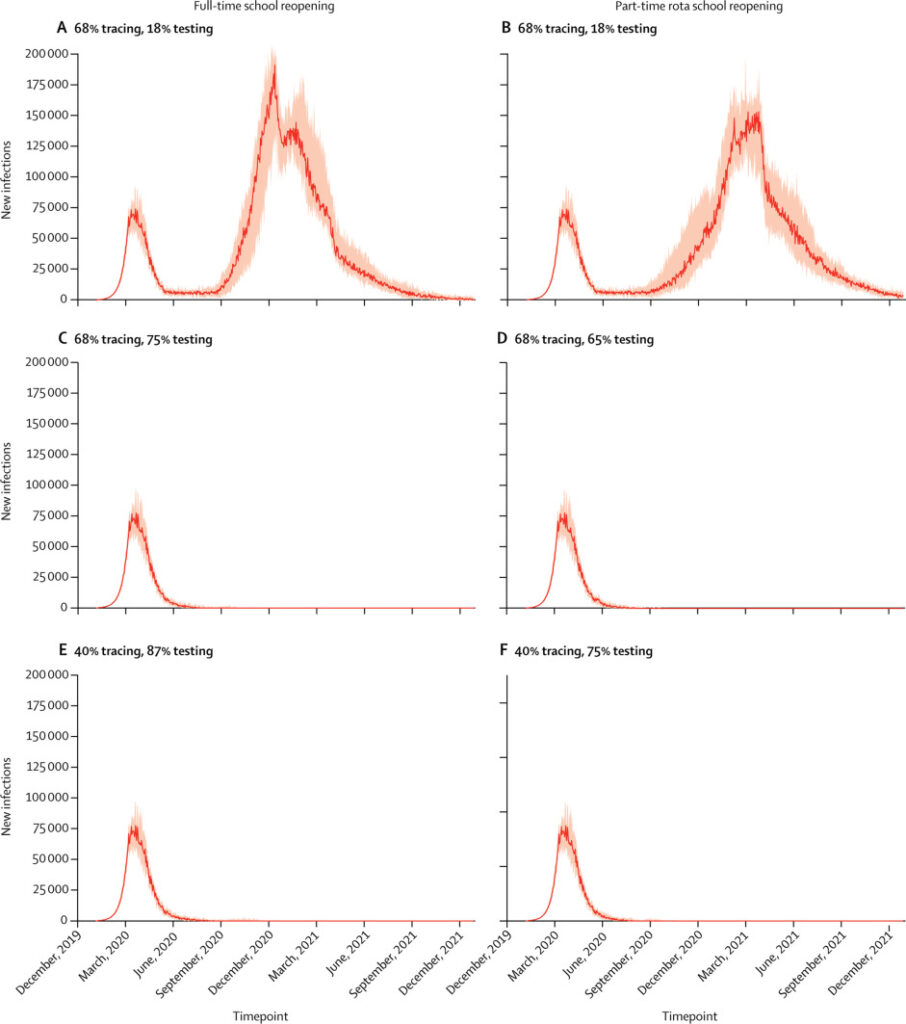
- A modeling analysis found that periods of strict social distancing followed by a robust level of testing, contact tracing and household quarantine could keep the disease within the capacity of the healthcare system while enabling the reopening of economic activities. A similar model from the UK found that assuming 68% of contacts could be traced, 75% of individuals with symptomatic infection would need to be tested and positive cases isolated if schools return full-time in September, or 65% if a part-time rota system were used. However, without these levels of testing and contact tracing, reopening of schools, together with gradual relaxing of the lockdown measures, are likely to induce a second wave that would peak in December 2020.
- A study of 1,000 children who tested positive found that minority children had a higher rate of infections (46% of Hispanic and 30% of Black children tested positive, compared to 7.3% of white children).
- The New England Journal of Medicine criticized the state-by-state approach in the spring. “Infectious diseases may not recognize political boundaries, but disease control policies certainly do,” the authors wrote. “Yet state or regional isolationism is a poor substitute for national leadership in pandemic response.”
- Researchers in South Korea found that roughly 30 percent of those infected never develop symptoms yet probably spread the virus, but they have a high viral load. According to The New York Times, “The study found that presymptomatic patients did not develop symptoms until 15 days after first testing positive on average; the range for most subjects was 13 to 20 days. This is highly concerning. Previous studies have reported that 95 percent of presymptomatic patients develop symptoms by Day 11. If the data from this study are accurate, it could mean that individuals might be spreading the virus unknowingly for far longer than we have previously realized and that 14 day quarantines suggested by the Centers for Disease Control and Prevention might be inadequate.” Asymptomatic people became virus-free a little sooner — around Day 17, compared with Day 19 or 20 for those with symptoms.
- One study found the same viral load in children and adults, and another found a correlation with viral load and mortality (those with a higher viral dose were more likely to pass away from the virus).
- For those who believe kids are “almost immune” to the virus, a study found one-third of kids who tested positive and were in the hospital ended up in the ICU.
- The New England Journal of Medicine lauded New Zealand for its successful elimination of Covid-19.
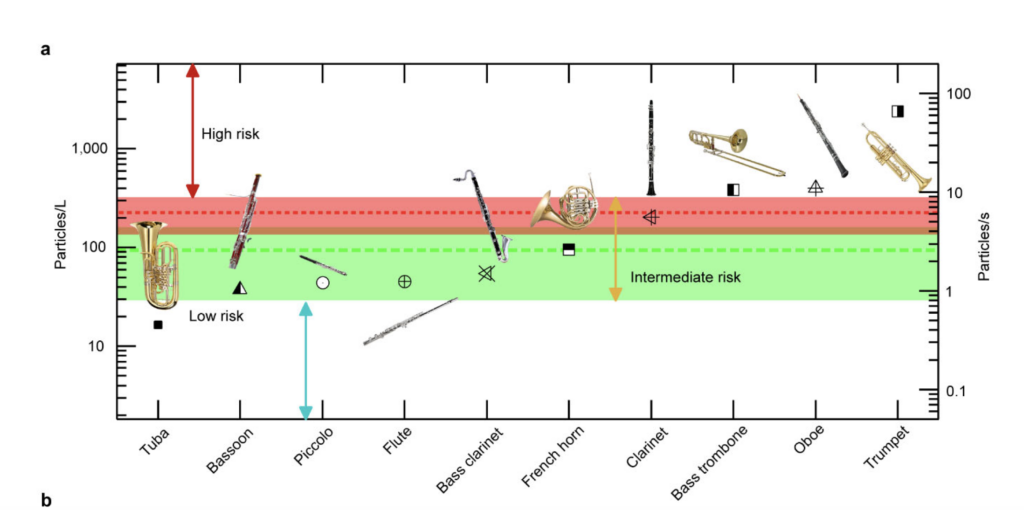
- In what could possibly be the greatest graphic ever published in a medical journal, researchers found that the tuba was the woodwind instrument that generated the lowest amount of aerosols.
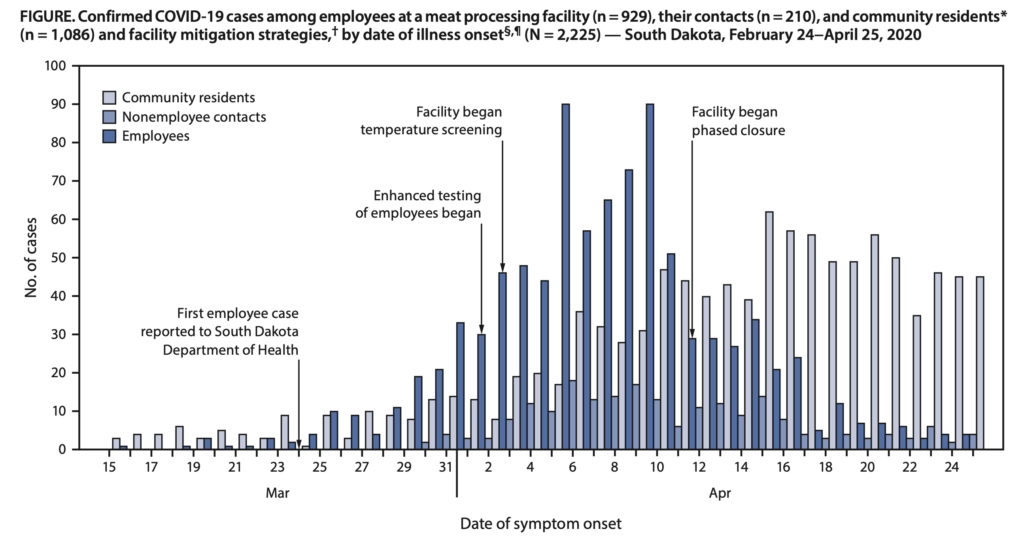
- A CDC report found that during March 16–April 25, 25.6% (929) of employees at a meat processing facility in South Dakota and 8.7% (210) of their contacts were diagnosed with Covid-19; two employees died. The highest attack rates occurred among employees who worked less than 6 feet (2 meters) from one another on the production line. While the closure in mid-April curbed infections, there was still community spread.
Let’s also take a look at developments around the world.
- The city of Melbourne has been placed under a near-lockdown as hundreds of new cases were detected.
- Japan is currently experiencing a series of new infections.
- Financial evidence shows that widespread mask wearing in China has also reduced transmission of cold and flu viruses, with drugmakers reporting plummeting sales of cold and flu medication this year.
- At least 40 people have been infected with Covid-19 on a cruise ship in Norway. (What did we learn about cruises and the coronavirus?)
- Israel’s reopening of schools and releasing restrictions too early serve as a cautionary tale.
- Germany is now testing all incoming travelers from “hot zone” areas.
- As VICE’s Sammy Westfall reports, a military-style lockdown in the Philippines will not work by itself to curb infections.
- New Zealand has had 100 days without a locally transmitted case.
Finally, a quick update on vaccines. As Novavax’s vaccine shows encouraging results in Phase 1 trials, scientists worry about political influence over the vaccine project, especially with the possibility of Trump using the election to instill market confidence through the release of a vaccine. Evidence is needed that vaccines will be effective and safe. But even if a vaccine is effective, it is not a panacea. You must never abandon the public health response, Dr. Fauci said at a Brown School of Public Health forum on Friday, as reported by my colleague Cate Ryan. “You should think of the vaccine as a tool.”
The IHME model has now raised its prediction to 295,011 deaths by December 1.
Previously on July 31, the model predicted 230,822 deaths by November 1. Universal mask wearing (95% of the population) could lower the predicted death count by 70,000. IHME modelers outlined three scenarios: staying the current course and facing 300,000 deaths, states reimposing mandates in the fall due to a surge in cases, or universal mask wearing to save 70,000. I trust Americans will pick the right path.
Having laid down the groundwork on the national scene, let’s take a look at the latest developments in higher ed.
Higher education
This week, I launched an updated version of my “Flip Tracker,” an interactive map tracking colleges’ changes to their fall plans. According to the tracker, 126 schools have announced changes or reversals to their fall plans. While many shifted all courses (or most courses) online, many have delayed the start of their semesters by a few weeks, some as a result of state restrictions. You can browse the map here.
Most schools (100) have referenced the ongoing public health situation (either on the state or national level), while many (43) have said community health and safety as a reason for their change. A small group (27) have said that state regulations caused them to move courses online (current regulations in New Jersey do not allow for in-person classes). Some also cite testing availability or turnaround issues as reasons for their change.
After a handful of colleges in New Jersey moved online due to state regulations, Princeton University surprised the higher ed world on Friday afternoon with their announcement to move all courses online for the fall. In its statement, the university’s president said that “People throughout this University have done outstanding work to prepare the campus to receive students safely, but the risk of widespread contagion and serious illness remains. Moreover, even if we successfully controlled on-campus spread of the disease, transmission rates might rise statewide or in our region.” This is noteworthy — I have long said that higher ed cannot exist in a vacuum, and it seems that this has rung true for Princeton. In an incredibly well-written letter to the college community, Smith College, a small rural school in Massachusetts, attributed four factors to its decision to be remote for the fall:
- “Troubling new phase” of the pandemic
- Increased transmission rates
- Potential for rapid asymptomatic transmission
- Failed school reopenings in other countries
“We have a civic duty to the communities in which we live and work.… As critical as higher education may be, none of us wants it to be the driver of a second wave of virus transmission in our host communities,” Smith’s president said.
In my opinion, the most significant school flip was that of Johns Hopkins University, who moved all courses online for the fall. Speaking to The Chronicle of Higher Education’s Lindsay Ellis, Dr. Tom Inglseby, one of the university’s top infectious disease specialists, said that despite the university’s rigorous twice-weekly testing strategy, it’s an “incomplete defense.” “Even if you test every single student on Day 1, that test only tells you that they’re negative on Day 1,” he said.
It is unclear how much of a factor is Baltimore’s inclusion on Dr. Birx’s nine cities to watch list played into Hopkins’ decision. However it begs the question, if Hopkins can’t reopen safely, with its large endowment, twice-weekly testing strategy and the best public health experts in the country, who can?
Testing remains a critical element for colleges to reopen safely. Researchers at Caltech have compiled an excellent database of college testing plans; I have joined with them in their analysis and we will be publishing a manuscript preprint shortly, in time for next week’s report. Testing protocols vary widely. As the University of Illinois plans to test all students twice per week, Boston University is employing robots to run their labs, and other schools will only offer testing for symptomatic individuals. This is not sufficient. Surveillance testing of entire populations will be necessary to most effectively curb infections.
As the school year approaches, professors who have had recent social distancing teaching experiences have warned their peers that people rely on visual communication cues more than they realize, and masks or seating arrangements may inhibit those. HyFlex (having in-person students interact with others on Zoom) is difficult, two professors wrote in Inside Higher Ed. Many have called for dramatic improvements to remote learning. In one op-ed, two instructors called for the need for culturally relevant and timely pedagogy. “What if college and university presidents saw this September not only as a campus emergency of epic proportions but also as an astonishing educational opportunity — a fall like no other, but in a good way?” they said.
Meanwhile, at Boston University, faculty were given a playbook on how to communicate with their students about the upcoming semester, according to reporting from my colleague Grace Ferguson. “Keep it positive,” it said. “Focus on the innovative features of your courses…on the great educational experiences you expect your courses to deliver.” The letter also encouraged faculty to avoid using the word “online,” instructing them to say that courses will be delivered “remotely.” This letter also just happened to come on the week that tuition deposits for the university were due, underscoring the value that tuition provides to colleges and showing why some are not decreasing tuition for online courses (I discussed some of these dynamics in an interview with Kevin Gaiss at WCAX, Vermont’s CBS affiliate).
As colleges begin to bring students back to campus, it is clear how much of an epidemiological shock mass movements of students could bring to the nation’s coronavirus response. The Chronicle of Higher Education conducted a visual analysis of all first-time students and showed that many of this population of 400,000 are coming from states with high levels of disease prevalence. I conducted a similar analysis, this time focusing on five schools in the NESCAC in New England: Bates College, Bowdoin College, Connecticut College, Middlebury College and Tufts University. Of the total of 12,348 students, 20% (2,443) live in states designated by the White House to be in the “red zone.” Multiply this by thousands of colleges nationwide and you can see how much of a shock this could cause to disease spread.
Despite all this, the majority of students will return to college campuses, if their colleges will let them. While 20% of Harvard first-years have deferred matriculation to the following year, 78% of University of Pennsylvania students surveyed by The Daily Pennsylvanian intend to return to campus for the fall semester. According to reporting from my colleague Pia Singh, the academic experience, social life and mental health are the three major factors that driving Penn students to return (it remains unclear what socially distanced social life will mean). Physical health and family influence have driven some students not to return.
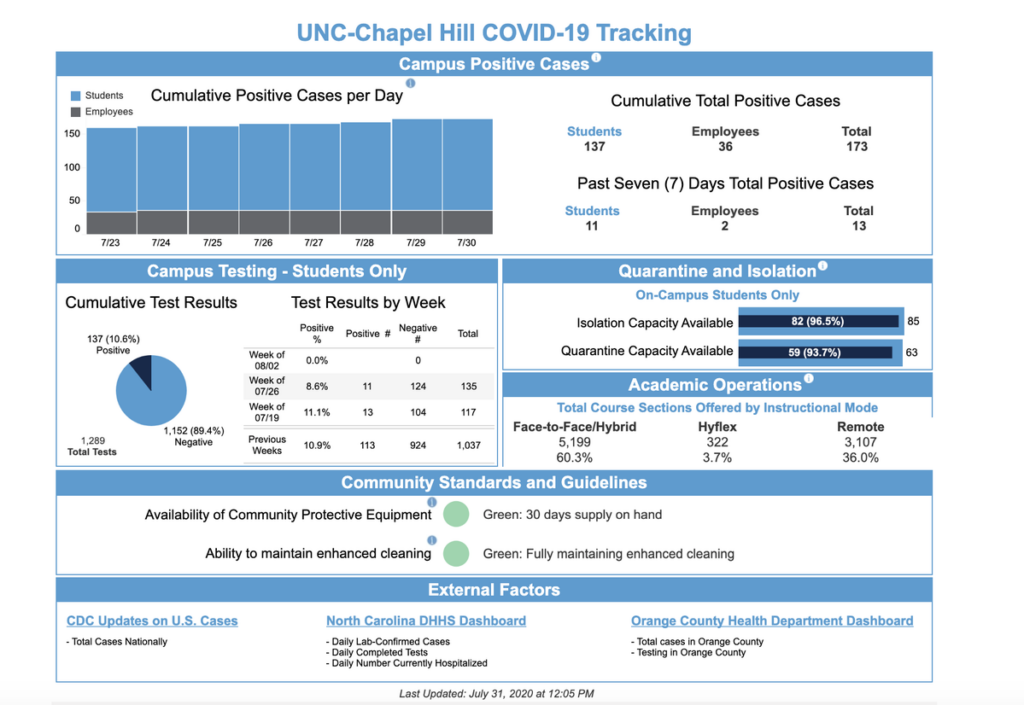
For those who do return to campus, colleges must be prepared to be transparent about their case counts when tests come back positive. As reported by my colleague Piper Hansen, Arizona State University does not intend to report cases in the college community, instead referring those to the state’s health department to search for the cases in the college’s ZIP code. “Knowing how many cases may be present in our community at one time does not give members of our community useful information about whether they particularly may need to take extra precautions,” a university spokesperson said. This is ridiculous. Check out the University of North Carolina’s dashboard as a comparison. Colleges should be prepared to report these statistics.
Each week, we take a moment to acknowledge the wackier elements of colleges’ reopening plans, also known as the College RidicuList.
- At Villanova University, each student will be provided with a portable outdoor chair for classes.
- At Indiana University, the school believes taped X’s on chairs will accomplish social distancing.
- Students at Jones University will wear wristbands when they have completed health checks.
- Oakland University has recommended that students wear a “BioButton” to monitor for Covid-19 symptoms (this is extra ridiculous).
- An innovation team at Middlebury College put together a video with suggestions for socially distanced social life, which includes creative items such as “DIY telephones,” “themed tents” and “cloud watching.”
- Officials at Syracuse University have likened their quarantine to a “minimum-security prison” (their words, not mine) and have already suspended students for breaking quarantine protocols.
On the athletics front, the Mid-American Conference was the first major conference to suspend its fall season, as Big 10 and Pac-12 football players called for better safety protocols. The NCAA has suspended Division II and Division III championships. At this rate, it is a matter of time until most athletic competitions at the college level will be suspended. My tracker has recorded 956 cases in college athletics programs so far.
Here are some samples from op-eds and editorials in student newspapers this week, which are always useful for capturing perspectives from students, faculty, staff and local community members.
- “Stanford has trapped RAs in an uncomfortable position,” one resident assistant at Stanford said. “We want to be there for our residents, but the University is demanding our commitment before telling us what risks we will be assuming or what to expect from the job.”
- “Moreover, there is no pedagogical benefit, in my courses and many others, to socially distanced in-person instruction,” one faculty member at Boston University said.
- “The seniors and other vulnerable populations who live in these neighborhoods must not be put at such elevated risk,” a Boston city councilor said about Northeastern University’s fall plans.
- “The more we deny the reality of the situation, the longer we drag this on,” one Arizona State University faculty member said.
- Local health officials in Chapel Hill called for the University of North Carolina to go online for the first five weeks of the semester. “The University will continue to regularly advise and consult our partners at the [Orange County Health Department] as we navigate the days and weeks ahead,” the system’s chancellor said in response.
- “I’m deeply satisfied to be at a place that views and values me as a human, not as an expendable CV,” one Bowdoin College faculty member told my colleague Kate Lusignan on Bowdoin’s plan to only bring back first-year students.
Student behavior still remains a wild card. A paradox seems to exist between students trusting themselves to do the right thing but not trusting their peers. Check out these results from a University of Iowa survey.
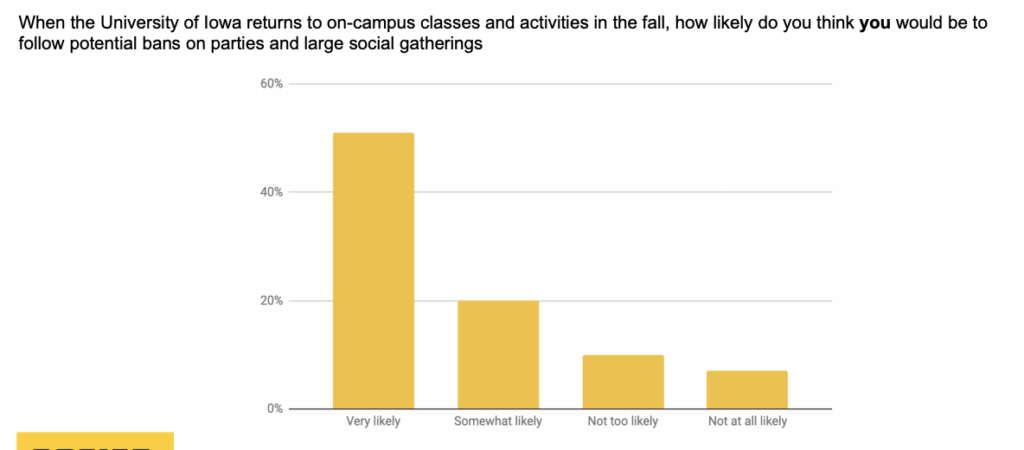
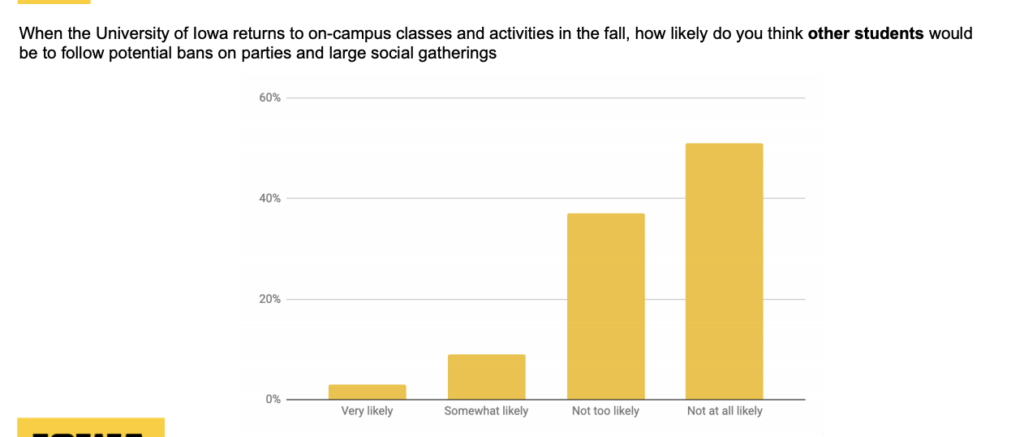
Some colleges have acknowledged the risk of bringing students back to campus. Others are choosing to deny it. “If you can live safely and study successfully at home, we encourage you to consider that option for the fall semester,” Michigan State University president Samuel Stanley told students. Football players and university athletic department staff at Colorado State University (CSU) say coaches have told players not to report Covid-19 symptoms, threatened players with reduced playing time if they quarantine, and claim that CSU is altering contact tracing reports to keep players practicing. Upon move-in and after testing 3,000 people, Iowa State University found 66 positive cases, many of whom will isolate on campus. Southern Methodist University’s plan calls for students to quarantine with their roommates if they are contact traced and even says that students may have to isolate at home (potentially infecting others) if isolation spaces are filled. This comes as the university says that it will only administer around 50 tests per day. It’s worth noting that a Cornell University report found that the average number of contacts on a campus could include anywhere from 8 to 17 people per day. Few colleges have publicly set thresholds to shut down their campuses.
So where do we go from here? It’s already the beginning of August. In my opinion, most colleges who will reverse their fall plans have done so already. In a matter of days, students are moving in. It is possible that schools that start later will look to others who have experienced outbreaks and be tempted to change their plans. I also question what will happen if there is a worsening national or local pictures in the coming weeks. The country’s progress could quickly be eliminated if the public is not careful. Going into the fall, I worry about three major issues:
- What will student morale on campuses be like once students start falling ill?
- How disruptive will quarantines be once contacts are traced and students may be in and out of online classes?
- What will be the effects of a giant mass exodus for Thanksgiving?
Higher ed is once again at a crossroads. As some hold fast to their reopening plans and other decide to reverse course in the best interest of the nation, we mourn the loss of a University of Georgia employee due to Covid-19. Unfortunately, it is possible we may see similar tragedies in the weeks and months to come. “If colleges go ahead, they will endanger the lives of students, staff, faculty, and those who live in the surrounding communities,” Yascha Mounk writes in The Atlantic. “Reopening colleges is the wrong thing to do.”
Study abroad and international travel
It is clear that travel and immigration restrictions have already had an effect on incoming first-years, as the international students’ orientation at the University of Notre Dame had 200 fewer students than in previous years. The State Department has lifted its global travel warning it placed on March 19, transitioning to country-by-country restrictions. This does little to the study abroad market for the fall, as there are still many other hurdles to program operations. In a blog post, William Gertz, president of the American Institute for Foreign Study (AIFS), said that in a post-pandemic world, study abroad will be more important than ever. “Globalization is not over just because borders are closed,” he wrote. “In fact, the pandemic has made it crystal clear how important it is for teams of people around the world to be able to work together toward a solution that everyone on the planet benefits from.”
The Good Stuff
Let’s roll the clips of the good stuff. In my usual tradition, I feature my favorite stories from the week. Here are my Top 10.
- Chris Rogan is a miracle man. The 29-year-old patient had to be intubated twice for a total of 71 days, put in a coma for 61 days, coded once, had a tracheotomy and suffered blood clots that resulted in a bedside leg amputation. After spending 132 days in the hospital, he was finally discharged this past week.
- Astronauts Bob Behnken and Doug Hurley returned to Earth on SpaceX’s Crew Dragon in the first water landing by an American space crew since 1975.
- A semicolon helped The Atlantic’s Ed Yong write a 212-word sentence in his article, “How the Pandemic Defeated America.”
- Dr. Anthony Fauci’s neighbors celebrate him as a hero with signs and gratitude.
- My colleagues Leah Abrams and Jake Satisky helped spearhead an amazing project in partnership with the Poynter Institute to showcase college journalism covering campuses during the pandemic.
- Duke University’s student government was praised for its handling of the pandemic and transparency with the administration.
- The Washington Post ranked 14 brands of tortilla chips. In case you’re wondering, Santitas is #1.
- NPR interviewed Kermit the Frog on his upcoming Disney show.
- Olympic swimmer Katie Ledecky balanced a glass of chocolate milk on her head while swimming. And that’s not even in the top 5 of impressive things she’s done.
- CNN’s fantastic new documentary, “On the Trail,” features 10 women covering the 2020 primary season.
Conclusion
“Unless Covid is defeated everywhere, it won’t be defeated anywhere,” New York Governor Andrew Cuomo said this week. As the U.S. approached 5 million confirmed cases (and many more undetected), we must realize that every death from now on is preventable. In the absence of a national strategy, we must pledge as a nation to do everything we can to stop the virus’ spread. I fear that the return of K-12 schools, colleges and universities will bring an epidemiological shock that will cause the United States to spiral into an out of control outbreak this fall. It doesn’t have to be this way. Let us augment testing significantly (using antigen tests as a screening tool), conduct effective contact tracing and utilize social distancing and mask wearing to our advantage. The onus is on all of us. The word “pandemic” comes from the Latin roots “pan” and “demos.” All people. All of us.
I’d like to thank all the student journalists with whom I have the pleasure of working. In the next weeks and months ahead, they will become ever more important in chronicling their colleges’ paths forward for the fall and beyond. Support their work by reading it.
My best to all for good health.
Like what you see? Don’t like what you see? Want to see more of something? Want to see less of something? Let me know in the comments. And don’t forget to subscribe to the weekly newsletter!
For more instant updates, follow me on Twitter @bhrenton.


