Welcome back to Week 16 in my weekly reports analyzing the Covid-19 pandemic and its effects on the country, higher education and study abroad. For those of you reading this on my blog, Off the Silk Road, I have also launched a newsletter, where these reports can be sent directly to your email each week. Click here to subscribe.
Last week, we discussed two plans by Drs. Peter Hotez and Leana Wen to reset the national strategy and suppress transmission nationwide in order to safely reopen schools and colleges. This week, we will continue to look at more plans for a national reset and examine testing as our only key to open colleges.
There’s a lot of material to go through (as per usual), so let’s get straight to it.
A national look
It has been six months since I left China as a result of the coronavirus outbreak, and while China and many other countries have returned to some sort of “normal,” the U.S. most definitely has not. We have entered a new dangerous stage of the pandemic. While cases are not at their all-time record highs and many hotspots have stabilized, we are still recording 67,000 cases per day, hospitalizations are still high and Florida still has 9,000 new cases per day. This phase is dangerous because without record-high numbers reported in the media, I fear that the public will remain complicit and we could see another spike in the near future. July was the worst month in America’s battle against Covid-19. As deaths keep rising, sadly we are now seeing close to 1,400 people lose their lives every day. We are not in a good place.
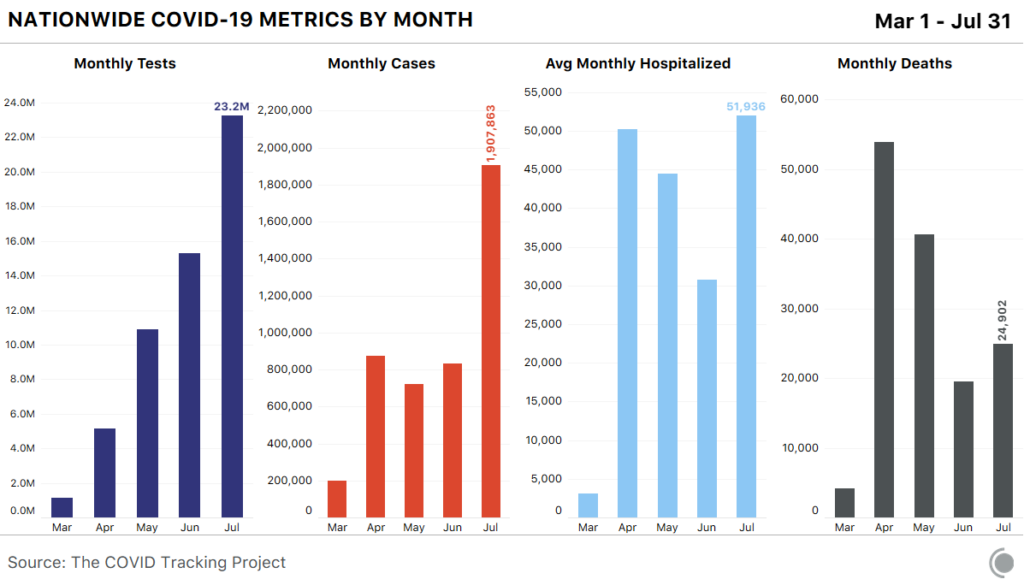
The virus has moved away from the South and West and has now moved inland. New states of concern include Ohio, Indiana, Kentucky and Tennessee, among others. Dr. William Haseltine, chair and president of ACCESS Health International and former professor at Harvard Medical School, says that there are now five areas we must specifically target in order to control the virus.
- Young people going out to party
- Workers in unsafe conditions
- Minorities in close contact situations
- Elder care and correctional facilities
- Schools
This week we have seen some high-profile Covid-19 cases: National Security Advisor Robert O’Brien, Representative Louie Gohmert of Texas and at least 20 players on the Miami Marlins baseball team. The Marlins outbreak shows that sports cannot be played safely unless they are in a complete bubble (similar to the NBA) and also further underscores the fact that this nation’s viral transmission rate is out of control. As a nation, we made the wrong choice. We focused on opening sports, rather than opening schools. Per reporting from Annie Grayer at CNN, 60 out of the nation’s 101 largest school districts will start the year online. As epidemiologists across the country are divided on whether or not to send kids back to school, one metric remains clear: community transmission must decrease in order for schools to open. The New York Times published a map showing that large parts of the country would likely see infected students if classrooms opened now. And in one case, it already has: at a school in Indiana that opened on Friday, one student tested positive and others were quarantined within hours of starting school. Schools can do their best to minimize transmission through modifying aspects of the school day, as seen in this graphic.

However, questions on reopening plans remain unanswered. Schools need to plan for appropriate actions for when cases are detected. In the case of New York City, one confirmed case will result in an investigation and the classroom will be closed for 14 days. While lower case counts and infection prevalence should be the factors driving schools to reopen, this does not appear to be the case; a Brookings analysis found that counties with higher levels of support for Trump were more likely to open in-person. If we can’t keep our millionaire baseball players safe, then how can we keep our kids at school safe?
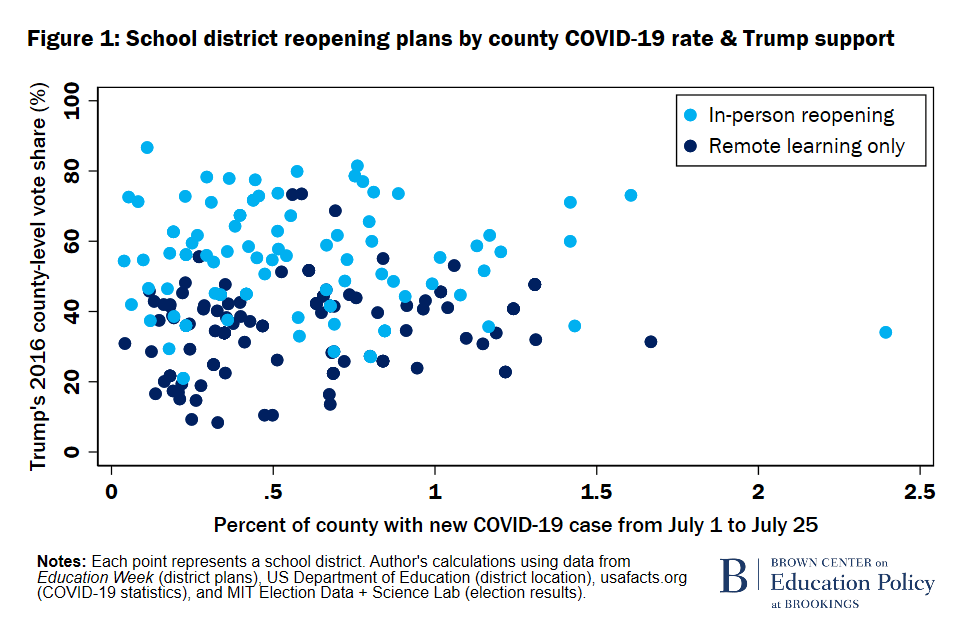
As our nation battles many simultaneous outbreaks and we lose one American every minute, the IHME model at the University of Washington has raised its predictions by 11,000 to show 230,822 deaths by November 1. This week, we surpassed 4.5 million confirmed cases and 150,000 deaths. Universal masking will lower the death predictions to 198,831. We still lack a national testing strategy as Jared Kushner has not pulled through (did anyone expect him to?). The turnaround times of test results are inconsistent across the country; in New York, it took me 15 days to receive mine.
We also face another crisis: misinformation and disinformation. It is hard to believe that this week was the week when “doctors” pushed the drug hydroxychloroquine in a viral video on the Internet. The overwhelming scientific evidence shows hydroxychloroquine is not effective as a treatment for Covid-19 and Dr. Stella Imanuel, one of the “doctors” in the video, believes in alien DNA and demon sperm. President Trump has embraced her message and Vice President Pence even met with some of the “doctors” in the video. And no, Mr. President, as my colleague Adrienne Dunn points out in USA Today, testing does not lead to more cases.
As usual, more studies have been published and new information is now available to help us better understand Covid-19. Let’s take a look at some of the highlights:
- A case study from a summer camp in Georgia, which required tests for campers prior to arrival and did not mandate the wearing of masks for campers, found a viral attack rate of a staggering 44% after three days and 26% asymptomatic infections. This has major implications for schools and colleges.
- Masks may reduce one’s viral dose and may even protect you from contracting the virus.
- A new paper in Nature shows that the virus originated from bats in China.
- A study from a plane in Wuhan shows transmission may have occurred during the flight. However, the majority of 16 cases in the outbreak were not attributed to transmission on the flight. Seating position is key; those who sat near the confirmed cases were more likely to be infected.
- There was an outbreak at an Israeli secondary school after students were allowed to remove their masks during a heatwave. Roughly 10 days after Israeli schools fully reopened on May 17, two students at a secondary school in Jerusalem were diagnosed with Covid-19. The resulting outbreak infected 153 students and 25 members of staff. By mid-June, a further 87 cases had occurred among the close contacts of people infected.
- Cats and dogs are just as likely to be infected with Covid-19 as people are, according to a survey in northern Italy.
- Modeling from the Diamond Princess cruise ship shows that airborne transmission was a major driving factor.
- A study shows that kids (less than 5 years old, 5-17 and 18+) have the same amount of viral load as adults.
- A new RT-LAMP testing strategy was evaluated. This is an outdoor, mobile assay with self-collected saliva and results in hours. Testing results were 100% concordant with qRT-PCR, with all but 1 person testing negative.
- A study in The New England Journal of Medicine shows that self-collected swabs (tongue, nasal, and mid-turbinate) perform nearly as well as professionally administered NP swabs, and may actually have even higher viral titres. This means that individuals can administer their own tests and it would be just as accurate.
- A new study shows the average time a person sheds the virus is 17 days.
- An analysis shows that primary and secondary school closures in March nationwide were associated with a −62% relative change in Covid-19 incidence per week and a −58% relative change in mortality per week.
- Research in the Southern Hemisphere shows that flu season could be reduced this fall due to increased mask-wearing behaviors, though further evidence is mixed.
- Rhode Island, a state that has been lauded for its coronavirus response, saw encouraging results: only 0.6% of the surveyed population has tested positive for antibodies.
Let’s also take a look at developments around the world.
- The New York Times asked young people from around the world to respond to America’s handling of the coronavirus. They were not impressed.
- China has seen an outbreak in the northwestern region of Xinjiang.
- North Korea recorded its first confirmed case.
- Europe (Belgium, Spain, France and Germany in particular) is facing a second wave.
- Tokyo and Hong Kong are dealing with a spike in infections.
- U.S. citizens are barred from traveling to most of the world.
So yes, this virus is not going anywhere. But here in the U.S., we can get our infections down to a lower baseline, which would enable us to better adopt a risk management approach in order to return to some semblance of normalcy.
We’re in this for the long-haul — Google has asked its employees to continue working from home until summer 2021. A poll from the Kaiser Family Foundation shows that more Americans believe the worst is yet to come. The economy is in shambles, contracting 32% this past quarter.
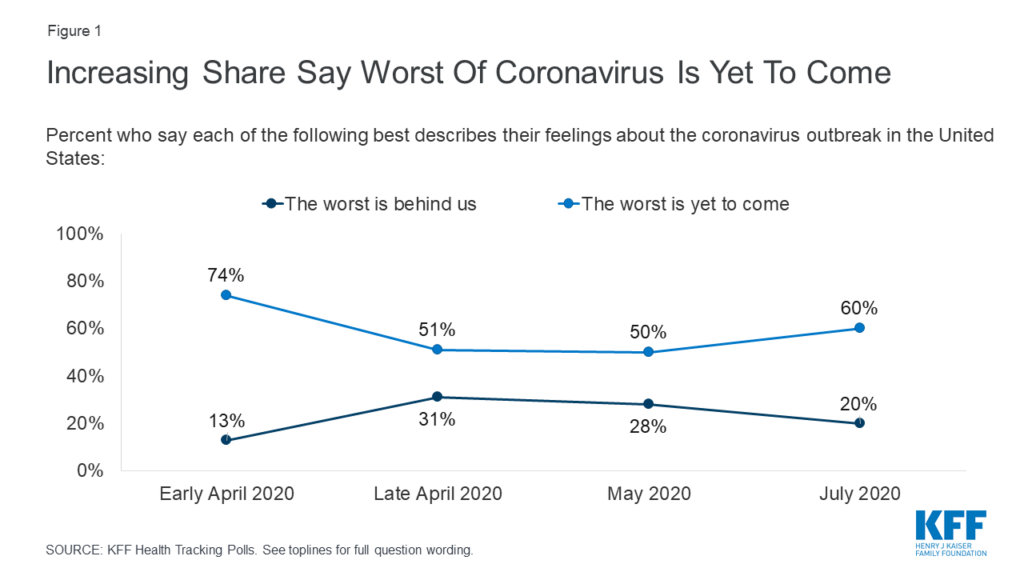
How do we get out of this? First, let’s discuss testing. Pooled testing, which was approved by the FDA last week, is useful in areas with low infection prevalence (in areas with high prevalence, pooled testing actually uses more tests as there is a higher chance of individual tests coming back positive). Multiple types of tests, even those that are slightly less accurate, can be used. XPRIZE Rapid Covid Testing, led by cancer startup CEO Jeff Huber, is a $5 million dollar, 6-month competition to develop faster, cheaper, and easier to use Covid-19 testing methods at scale. These types of rapid tests can be developed in the next few months, with the goal by January to have a barrage of tests. The project is backed by companies such as Amazon, Google and Anthem. Additionally, the FDA has posted a new template for an at-home diagnostic test. “While the recommended sensitivity for these non-lab tests is lower than lab-based tests, the tremendous benefits of broader access to simple and fast testing options generally outweighs this risk,” the organization said. Color has received an emergency use authorization for a self-administered test, lowering the burden on healthcare workers. So yes, these tests are out there. But we need to wait a couple of months for these technologies to come onto the market.
Next, let’s discuss plans to reset. The Association of American Medical Colleges has put forth a plan with the following nine immediate actions:
- Remedy critical supply and drug shortages.
- Increase availability and accessibility of testing.
- Establish national standards on face coverings.
- Establish and enforce national criteria for local stay-at-home orders and reopening protocols.
- Establish national criteria for K-12 school reopenings and convene a working group to study different approaches.
- Immediately expand health insurance through COBRA.
- Begin planning now to prioritize distribution of the SARS-CoV-2 vaccine.
- Address and resolve health care inequities.
- Inform, educate, and engage the public.
The Association calls for 2.3 million tests per day, based on a goal of maintaining a positivity rate of below 3%, at the current rate of 70,000 newly diagnosed cases per day. For context, this week the U.S. conducted around 840,000 tests per day.
A plan put forth by the Johns Hopkins Center for Health Security includes these 10 components:
- Encourage and, where appropriate, mandate nonpharmaceutical interventions.
- Close higher risk activities and settings in jurisdictions where the epidemic is worsening and reinstitute stay-at-home orders where healthcare systems are in crisis.
- Bolster PPE supply chains and stockpiles and make information about the PPE manufacturing base and supply chain publicly available, with the goal of expanding PPE availability.
- Bolster test supply chains, plan for shortages, and collaborate with states and commercial laboratories to expand capacity and improve test turnaround times.
- Conduct and make public detailed analyses of epidemiologic data collected during case investigations and contact tracing.
- Curate and fund a rapid research agenda to cope with major challenges that have arisen.
- Scale up contact tracing and continue to improve performance.
- Identify and disseminate best practices for improving the public health response.
- Plan for a vaccine, including production, allocation, distribution, and community engagement, to ensure a successful rollout.
- Develop policies and best practices to better protect group institutions.
These plans are out there for the public to see. It is now a question of whether our leaders will do the same. Public trust in President Trump handling the crisis is diminishing, as seen in this poll of states in the Northeast.
Let’s finish today’s discussion with two final notes: disaster preparedness and vaccines. Florida’s state-run testing sites will close for four days this weekend due to the impending hurricane. This could be incredibly detrimental to the state’s coronavirus response. I am also concerned about hurricane shelters being potential breeding grounds for disease spread. Managing multiple disasters simultaneously is key to any emergency response.
Former CDC director Dr. Tom Frieden outlines three key hurdles to a vaccine:
- Will it work?
- Will it be safe?
- Can we get it to people?
However, he notes: “The biggest challenge to getting a Covid-19 vaccine into enough people’s arms won’t be scientific, technical or logistical; it will come from a lack of trust.” Outreach needs to start now. Once a vaccine meets efficacy requirements the FDA may issue an emergency use authorization within weeks, but this may not be until early 2021. Finally, global cooperation is necessary. This week, I attended an event hosted by the National Committee on U.S.-China Relations titled, “Lessons Learned Amid a Pandemic: How the United States and China can Collaborate on Global Health Crises.” Panelists, health officials in the U.S. and China, stressed the need for global cooperation in the weeks and months ahead.
Having laid down the groundwork on the national scene, let’s take a look at the latest developments in higher ed.
Higher education
A few weeks ago, I introduced the concept of the “Great American Flip,” where colleges would flip in succession to all online instruction. In many cases, this is happening, though not at the speed I would expect. While more complete data analyzing the reasons behind colleges’ decisions to move online will be available next week, I attribute the plans I’ve read to three major factors:
- State regulations
- Ongoing public health situation
- Testing availability
First, let’s discuss state regulations. Clearly, they are now having a huge impact on colleges’ decisions, specifically quarantine requirements. Georgetown University, George Washington University, American University and Catholic University of America all went online within a few days of each other, many citing the District’s quarantine requirement for 27 states. This “domino effect” is seen on a hyper-locality level — if one school goes online, their peers do so as well. In the case of Cornell University, New York’s quarantine order covers 34 states, and the university has announced it will no longer be able to provide quarantine housing; students returning to Ithaca from one of the 34 states on New York’s 14-day quarantine list must either find a place to isolate off-campus, or take courses online until their state is removed from the list. “While University administrators continue to affirm Cornell’s commitment to in-person learning for the Fall of 2020, key changes, demonstrative of a lack of preparation and a loosening grasp on campus public health measures, are being made,” the editorial board of the school’s student newspaper said. In San Diego and Los Angeles Counties, current guidelines do not allow for in-person classes. I have repeatedly stated that higher ed does not exist in a vacuum and must depend on the national picture. It seems that universities are finally starting to notice.
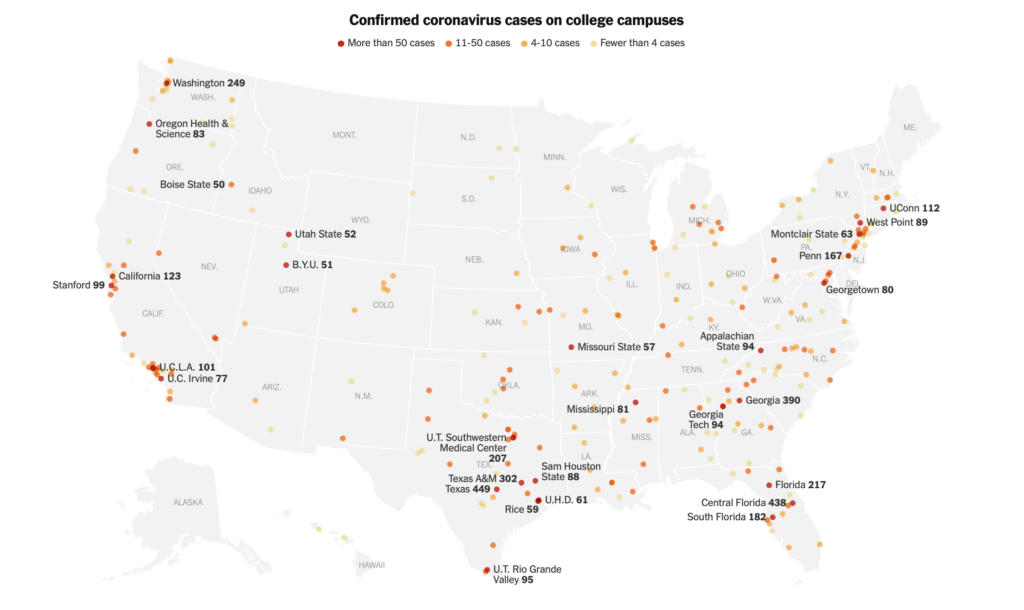
There was much chatter on the higher ed Twitterverse on this New York Times article linking 6,600 cases to college campuses. Many of these include those I have previously tracked in college athletics. However, this map is a gross undercount — both in terms of the way The New York Times sampled the schools (out of 1,000 they reached out to, only a few hundred responded) and the varying definition of a case. Is a student who tested positive after going home counted? How about an employee — who is affiliated with the college and lives locally, but may not have contracted the virus on campus? Similar to the Clery Act, which mandates that colleges be transparent around campus crime policy and statistics, we need a national standard to record cases and a national repository going into the fall.
Each week, we also take a moment to acknowledge the wackier elements of colleges’ reopening plans, also known as the College RidicuList. While some of these are rather humorous, others are rather intriguing approaches to public health. Hofstra University is selling air purifiers for students, with the claim that these machines filter 99.9% of Covid-19 particles (this is not proven). Tufts University is requiring those students who live out of Massachusetts’ quarantine-free states to test negative three times before they start the semester. Boston University may house vacant rooms in graduate student housing as quarantine spaces for students who have been exposed to confirmed Covid-19 cases. This just defeats the purpose of quarantine. Bowdoin College, which is bringing only first-year students back to campus, is providing every student with an iPad, at a cost to the college of $750,000 a year. Syracuse University has purchased 3.4 million masks, underscoring the cost of a Covid campus. The University of North Carolina at Pembroke encourages students to go home when they test positive, possibly further contributing to household and community spread. The University of Texas at Austin has forbidden all parties for the semester (good luck at this).
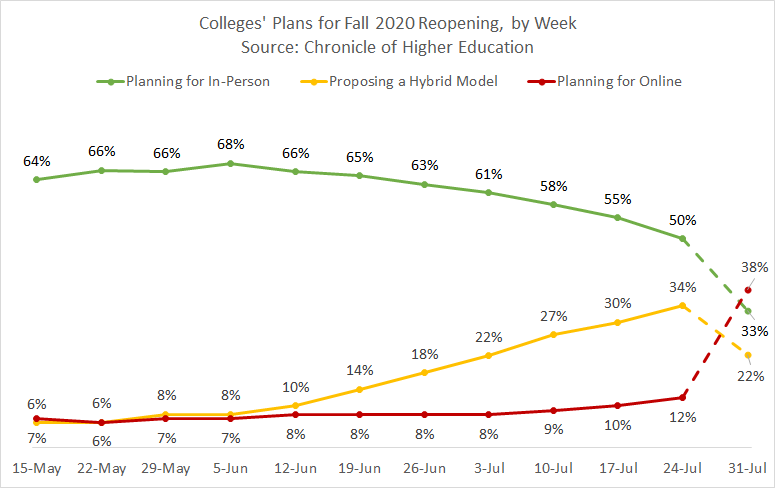
I am happy that The Chronicle of Higher Education has now chosen to use Davidson College’s College Crisis Initiative (C2i), headed by Chris Marsicano, to compile college reopening plans for the fall — the definition “hybrid” has deviated significantly from a few months ago. In the coming weeks, we will look to their data to analyze national trends. As seen on this graph, the number of institutions planning for in-person classes has decreased.
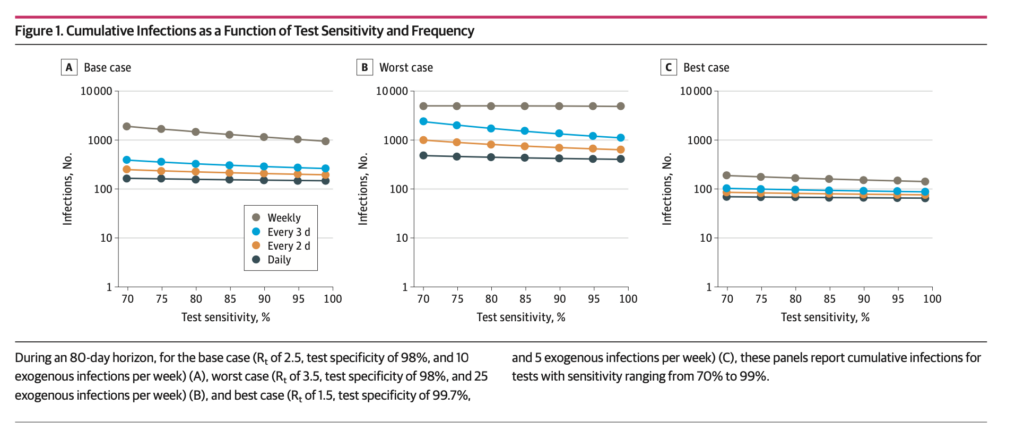
Testing, testing testing. I cannot underscore enough how important testing is for colleges to reopen. If a college does not have a frequent surveillance testing program, they are putting their communities at risk. This point was highlighted in two models this week: one out of Emory University and the other out of Yale University and Massachusetts General Hospital. The Emory model found that monthly and weekly screening can reduce cumulative incidence by 42% and 80% in students, respectively. The Yale model found that a rapid, inexpensive and poorly specific test will work if screening is conducted every 2 days. It uses a population of 4,990 students with 10 infections at the start of the semester. It’s worth noting that we discussed this model a few weeks ago when the paper was in the preprint stage. The model assumes test results are returned in 8 hours and students are immediately moved to isolation. This type of screening would only cost $470 per student per semester. Screening every 2 days resulted in 243 cumulative infections for the whole semester. Screening every 7 days resulted in 1,840 cumulative infections for the whole semester. Obviously, a highly specific test (with a low false negative rate) would be most ideal. However, the modelers found that frequency of screening had a profound effect on total infections, and specificity mattered less. Most importantly, symptom-based testing policies (ahem, UNC) do not work: “We identified no circumstance in this modeling study under which symptom-based screening alone would be sufficient to contain an outbreak.” Here’s a graph of how test sensitivity and frequency of screening affect cumulative infections. As you can see, frequency is key. If colleges want to even consider reopening, they must be prepared to test all students, faculty and staff frequently (ideally twice a week or every two days) and procure tests with fast turnaround times. Otherwise, it’s not safe to reopen.
Colleges need to be clear about their testing protocols. As my colleagues Arielle Gordon and Miriam Brown report, Colorado College will now be testing all students on arrival after previously saying they would not. The Brown Daily Herald’s Olivia George pressed college administrators on Brown’s testing plans and it seems that these answers are non-existent at the moment. Syracuse University will require all students to have proof of a negative test prior to their arrival on campus. If they are unable to be tested in their locality, the university will charge them $49 for a test kit. This high price precludes from students having access to testing. Testing before arrival should not be used as a replacement for testing all students on arrival. Just look at the Georgia camp case study. Campers and staff were required to obtain tests before arriving and the attack rate was still 44%.
So what do the students think? A survey conducted by the student government at the University of Texas at Austin showed that on a scale of 0-10, with 10 being always, students gave believing their peers not to hold gatherings with 10 or more people a ranking of 2.36/10. This shows seemingly minimal perception of adherence. It is vital for colleges to understand student behavior and conduct similar surveys.

Here are some samples from op-eds and editorials in student newspapers this week.
- “Our leaders are failing to protect and care for our community,” one Duke University graduate student said. “Duke’s decision to reopen could cost lives.”
- “By Bates’ own admission, coming back to campus poses a risk of serious injury or death,” a group of Bates College students, faculty, and staff said.
- “In five years, this fall’s return to campus will be remembered in one of two ways: it will either be a cautious gamble that paid off, or it will be the biggest mistake Middlebury College has ever made,” my colleague Jake Gaughan said in The Middlebury Campus.
- “If the school creates a culture where coronavirus doesn’t spread because of strict enforcement but everyone is really miserable and unhappy all the time, then why did we even invite people back to campus?” one Columbia University incoming first-year student said.
- “We wanted to make sure the message is getting across that the university should value lives over profit,” a Penn State graduate student said at a protest.
- One Emory University student wrote a controversial op-ed arguing for reopening, though I question its basis in public health and science, since he did not mention either. He argued that opening colleges will help herd immunity (we have learned that herd immunity is unattainable and may not last without a vaccine), young people are affected less (while they may be less likely to die they are still affected, and the long-term effects are unknown) and quotes Betsy DeVos (which is something one should never do when making actual public health decisions). So there’s that.
- “The plan is rooted in the wishful thinking that our students, for some reason, will act more swiftly than the citizenry of the majority of this country have to avert a coronavirus resurgence,” the editor-in-chief of the newspaper at Trinity College wrote.
- “Under current conditions, it is not safe for you to come to campus – to live in dormitories and apartments, to sit in classrooms, and to socialize with your peers in the way that college students usually do,” faculty at UNC said. This also comes as faculty at Columbia University have been pressured to teach in-person.
- Opinions of local residents are valuable as well. “Hanover wants you back, but not given the way students are currently conducting themselves which could well lead to a Covid outbreak,” the town manager of Hanover, New Hampshire, where Dartmouth College is located, wrote. “Smarten up, folks.”
- Staff values are vital. “If campuses reopen to students but most faculty teach remotely, students & admins who show up might see more clearly how staff are the connective tissue holding campus together—the cooks in dining, janitors cleaning residence halls, & techs maintaining digital infrastructure,” Jeff Selingo writes in The Atlantic.
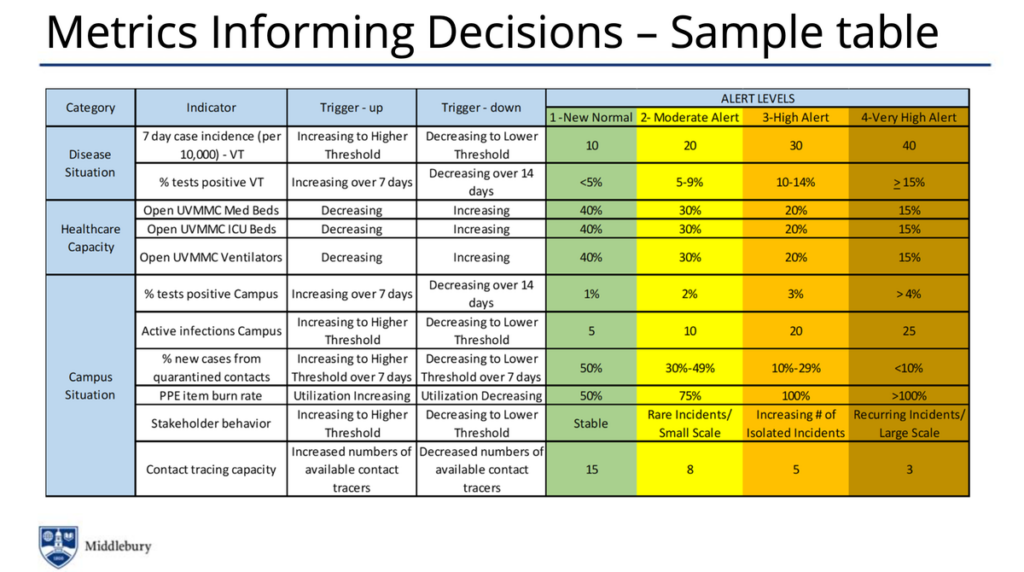
If colleges choose to open, they must set clear benchmarks for closing campus and an evacuation plan for students to leave if necessary. “We cannot repeat the chaotic situation in March,” I wrote on Twitter. In response to my comment, University of Illinois epidemiologist Rebecca Lee Smith wrote, “We don’t want to give a threshold to close because we want to be able to balance all the evidence – the problem with thresholds is that they can become requirements. If we see things going south, we want to be able to call it early.” In many cases, I agree with Dr. Smith. However, I would at least like to see assurance for students that they will know how to evacuate campus (Where do students store belongings? Will transportation be provided to airports?) before they set foot on campus this fall. Liberty University has said if more than 5% of students and employees present symptoms of the virus or test positive for it over a two-week period, then the university would shift to remote work and virtual instruction. With a student body population of 15,000 students, 5% would be 750. This is absurdly large. Syracuse University includes five “levels” of operation that lead up to a complete campus closure. If the university found more than 100 coronavirus cases and officials felt they couldn’t adequately contain the outbreak, the campus would come to a “pause.” All students would be confined to their rooms. I would also argue that 100 infections is rather large. By the time you detect 100 infections, viral transmission tells you that there will be more than 100 actual infections. While Middlebury College has not said what actions it will take, 10 active infections constitutes a “moderate alert” and 25 a “very high alert.” We need to see more examples of thresholds before students arrive on campus this fall.
I would also encourage colleges to look beyond the re-entry procedures and think critically how their plans will hold up in fall and winter, which depending on the climate, may invalidate many outdoor activities. Purchasing tents in Massachusetts for the fall will not work for students to eat outdoors in December.
As colleges consider the costs of flipping to online instruction, it is worth noting that a Brookings analysis found that movement to online education is unlikely to reduce instructional costs.
Finally, let’s check in on our map of confirmed cases in college athletics. As workouts and practices continue to be suspended due to confirmed cases, we have now tracked 850 cases across the country, more than the number of confirmed cases aboard the Diamond Princess cruise ship (712).
Will we see more colleges switch to online in the coming weeks? Yes, it is likely, but time is running out. We have also seen more schools delay the start of in-person classes. Ohio University, for example, will start in-person classes a month late, on September 27. Robert Kelchen points out that more schools will begin adopting this method as a way to buy time, and we could see them keep delaying the start of in-person classes if conditions worsen. Again, I cannot reiterate the importance of regular testing as a form of screening. This will act as a Covid-19 filter — enabling confirmed infections to be detected easily. UNC says that testing everyone “could create a false sense of security.” Where did they get that from? The CDC guidelines for higher education, which biologist Carl Bergstrom and many other scientists say are irresponsible. If Texas A&M spent as much money and time on testing strategies instead of producing promotional videos or “shared community values,” then maybe we would be in a better place to safely reopen campuses. No tests, no campus. It’s that simple.
Study abroad and international travel
Not much to report here on study abroad, as most programs have been cancelled for the fall. I was intrigued by this op-ed by Johns Hopkins professor William G. Durden in Inside Higher Ed. “An expanded notion of study abroad — one that includes immersive and direct engagement with people who practice international traditions and cultures within the United States, has the potential to elevate the field to a critical part of higher education pedagogy,” he wrote. I think this fall is a great time to rethink study abroad and introduce more international experiences into college curricula.
A new report from the Institute of International Education provides some new insights into how international students and study abroad will play out for the fall.
- Many international students were enrolled in the U.S. for the summer, though the report expects a slight decrease for the fall
- 38% of institutions are universally testing for Covid-19
- 64% have cancelled fall abroad programs (I am surprised that this number is not higher)
The Good Stuff
Let’s roll the clips of the good stuff. In my usual tradition, I feature my favorite stories from the week. Here are my Top 12.
- Ordinary people with extraordinary vision can redeem the soul of America by getting in what I call good trouble, necessary trouble,” civil rights hero and Congressman John Lewis wrote in a posthumous op-ed. “The vote is the most powerful nonviolent change agent you have in a democratic society. You must use it because it is not guaranteed. You can lose it.”
- U.S. News and World Report has launched Hospital Heroes, a series of profiles highlighting frontline healthcare workers.
- Students and alumni at the University of Vermont have continued to take care of 100 dairy cows throughout the pandemic.
- One high school editor in Portland, Oregon has garnered national attention for covering the city’s protests for months.
- The owners of a laundry shop in central Taiwan have become Instagram stars for posing in garments left behind.
- The Associated Press Stylebook says that “PB&J” is acceptable in all references to a peanut butter and jelly sandwich.
- A camp in Vermont for young cancer patients and survivors has adapted to form communities online.
- A writer at The Daily Pennsylvanian investigated why President Trump did not play sports at Penn, despite his claims of athleticism.
- Trump announced, then canceled, a Yankees pitch. Both came as a surprise to the Yankees and the White House.
- The team at The Daily Princetonian produced a wonderful interactive frosh orientation issue for Princeton’s first-year students.
- One Penn student describes working as an EMT in New York City this past spring.
- More than 500 photographers around the world took photos of people on their porches as a charity fundraiser.
Conclusion
We are still in an uphill battle against this virus. It continues to move inland, rising infection rates in new states. This is dangerous — without the public’s attention, we cannot be complicit. There is a dearth in data — under the Trump administration’s new hospitalization data reporting system, we still do not have a clear picture of how many people are hospitalized nationwide. Testing turnaround times remain abysmal. If colleges want to be serious about opening for the fall, they should be using testing as a way to do so. It’s the only way to ensure they have a shot at finishing the semester.
I’d like to thank all the student journalists with whom I have the pleasure of working. In the next weeks and months ahead, they will become ever more important in chronicling their colleges’ decisions for the fall and beyond. Support their work by reading it.
My best to all for good health.
Like what you see? Don’t like what you see? Want to see more of something? Want to see less of something? Let me know in the comments. And don’t forget to subscribe to the weekly newsletter!
For more instant updates, follow me on Twitter @bhrenton.


